After each of my 4 miscarriages, I had two lingering questions: Why did this happen? Was it my fault? During the long months of recurrent miscarriage testing, I also learned two things. Miscarriage is absolutely not the mother’s fault, and every doctor has different recurrent miscarriage workup protocols.
That’s why I compiled the information in this article. While basically every Reproductive Endocrinologist (RE) you see for recurrent miscarriage testing will do a blood workup looking for factors that could contribute to blood clots, there’s not enough continuity among practices in terms of other protocols.
This discrepancy among the tests doctors run, and the order in which they run them, stems mostly from the fact that there’s far less research into the causes of recurrent miscarriage than infertility in general.
And most REs specialize in getting people pregnant, not keeping them that way. So we never know if our doctor’s information is up-to-date. Having a guide to the tests different doctors are running allows us to advocate for ourselves as patients, which is essential when trying to decrease your risk of miscarriage.
Disclaimer: I am not a medical doctor. The information in this post is based on my experience and research. It is intended to help you communicate with your medical doctor and advocate for any tests you may not be offered. My suggestions do not replace the advice of your medical care team. No liability is assumed. Please read our full disclaimer.

This site contains affiliate links, meaning that we earn a small commission for purchases made through our site. We only recommend products we personally use, love, or have thoroughly vetted.
What Is Recurrent Miscarriage?
Recurrent miscarriage, often referred to as Recurrent Pregnancy Loss (RPL), is defined by the American College of Obstetrics and Gynecologists (ACOG) as a woman having 2 or more miscarriages .
Admittedly, this definition is a bit murky.
Many people consider 2 or more miscarriages “recurrent miscarriage,” but only if those two losses occur back-to-back and without the mother having previously birthed a living child.
If you’ve had 2 miscarriages without a prior positive pregnancy outcome, use this information to advocate for yourself to get treatment.
When Do I Qualify for Recurrent Miscarriage Testing?
The ACOG recommends a recurrent miscarriage workup after 3 losses. Some wonderful doctors and specialists are beginning to recommend a workup after only 2 losses, and I’m seeing more and more women have success advocating for testing after 2 losses.
Because different doctors have different feelings about tests and protocols, it may be up to you as a patient to advocate for yourself.
Moms in the US, whether you qualify after 2 or 3 losses may be up to your insurance company. Here are my 3 major suggestions for getting insurance companies on your side.
- Get your OB on your side first! They can talk to insurance companies in a way you, as an individual, cannot.
- Make sure your OB counts chemical pregnancies as losses. Because chemical pregnancies are so common, many doctors don’t count them in your miscarriage tally. But if you’ve had 2 losses and a chemical pregnancy, you can definitely make a case for having had 3 miscarriages. (In my book, a loss is a loss. Sadly, the insurance book is not mine.)
- Bring up other reasons you might need certain tests. The chances of getting your insurance to cover a hysteroscopy without meeting their criteria is low, but if you want blood tests for recurrent miscarriage (like factor v leiden, the lupus anticoagulant, etc.) you may be able to make that case. Show a family history of blood clotting disorders, stroke, or specific health issues, and your doctor may be able to code your tests so they aren’t related to miscarriage.
*Note: #3 is also a good option if your insurance won’t cover tests fertility-related tests!
I’ve Had 2 Miscarriages. Now What?
If you’ve had 2 miscarriages total, your OB will likely (though not necessarily) suggest you try again without intervention. If you’ve had a live birth between those two losses, I also recommend waiting.
The chance of miscarriage in any given pregnancy is estimated to be about 25%, so with a live birth in between, your chances of having an actual problem are still relatively slim.
The chance of repeat miscarriages is small—only 1% of women experience back-to-back recurrent miscarriage. By having back-to-back losses, you move into an altogether different, and much smaller category.
You know those “I am 1 in 4 memes” everyone shares around Pregnancy and Infant Loss Awareness Month? I’m so sorry, mama, but you’re now 1 in 100 just as these memes suggest.

After having two back-to-back miscarriages, 1 of 2 things will happen:
- Your OB will refer you to a specialist, likely a Reproductive Endocrinologist (RE)
- Your OB will tell you it’s “bad luck” and to try again. You can listen, if it feels right to you. If not, advocate for yourself!
What Are The Next Steps After 2 Losses?
The next step is up to you. Let me repeat that in case your doctor doesn’t make it clear. The next step is up to YOU!
Personally (and I realize my recommendation is colored by my own experience), I strongly recommend pushing for a full recurrent miscarriage workup after 2 back-to-back losses.
The chance of back-to-back miscarriages is low, which means the chance of there being some sort of problem is high.
That said, the chance of there being a problem is not as high after 2 losses as it is after 3.
Also, a recurrent miscarriage workup requires a lot of time, money, and energy. This is why many doctors suggest waiting, and why many RPL moms choose to wait.
Is A Recurrent Miscarriage Workup Necessary?
Not necessarily. About 65% of women who experience recurrent pregnancy loss can carry a healthy pregnancy with no medical intervention.
Basically, it’s a crap shoot.
Regardless of what’s causing your losses, each pregnancy is a new chance to have a successful pregnancy.
But if there is an underlying problem that leads to each pregnancy resulting in miscarriage, your chance of carrying a healthy pregnancy is slim. Testing is the game you play to find out if there’s a clear underlying problem if you should keep playing the odds.
Regardless of cause, the statistical facts remain. The odds are in your favor if you’re emotionally willing and physically able to play that game. The question is more about what your body, heart, relationship, and bank account can take.
What tests are in a recurrent miscarriage workup?
Recurrent miscarriage tests vary from doctor to doctor. Listed here are the types of tests you can expect, or advocate for if they’re not offered to you.
Before you begin testing, you should have a thorough meeting with your specialist where you provide a full gynecological history, including family history. Prepare all the information possible before that appointment.
Ideally, your doctor will conduct blood tests and anatomical evaluations based on your specific circumstances.
To be sure you get thorough treatment, download our printable recurrent miscarriage testing checklist. Take it with you to your initial appointment to be sure you get all the essential tests into your plan!
Why Give a Gynecological & Family History?
When you meet with a specialist for the first time, it will likely be a meeting. In this meeting, you’ll make a plan, but you likely won’t begin any actual testing. (Some doctors may choose to do blood tests on this day, but most will schedule it for later.)
This information will help your doctor decide which tests are most important for you, and in what order. Choosing tests in the right order can save you time, surgery, pokes and prods, stress, and a lot of money. It can also potentially give doctors ways to get your testing covered by insurance when it otherwise wouldn’t be.
Be warned: if possible, you’re going to have to ask your parents some potentially tough questions.
- Did they experience miscarriage?
- How many?
- Did their parents?
- Aunts and uncles?
- Has anyone in your family ever been born with chromosomal or physical abnormalities, such as Down Syndrome or a cleft palate?
- Do you have a family history of blood clotting disorders, heart disease, pregnancy complications, stillbirth?
If possible, you’ll need to ask most of these questions of your partners’ family, as well.
You won’t learn the exact problem my providing this information, but it could point your doctor in the right direction. For instance, if there’s a strong history of recurrent miscarriage on one side of the family, testing to see if you carry a chromosomal translocation becomes much more important.
List of Blood Tests for Recurrent Miscarriage
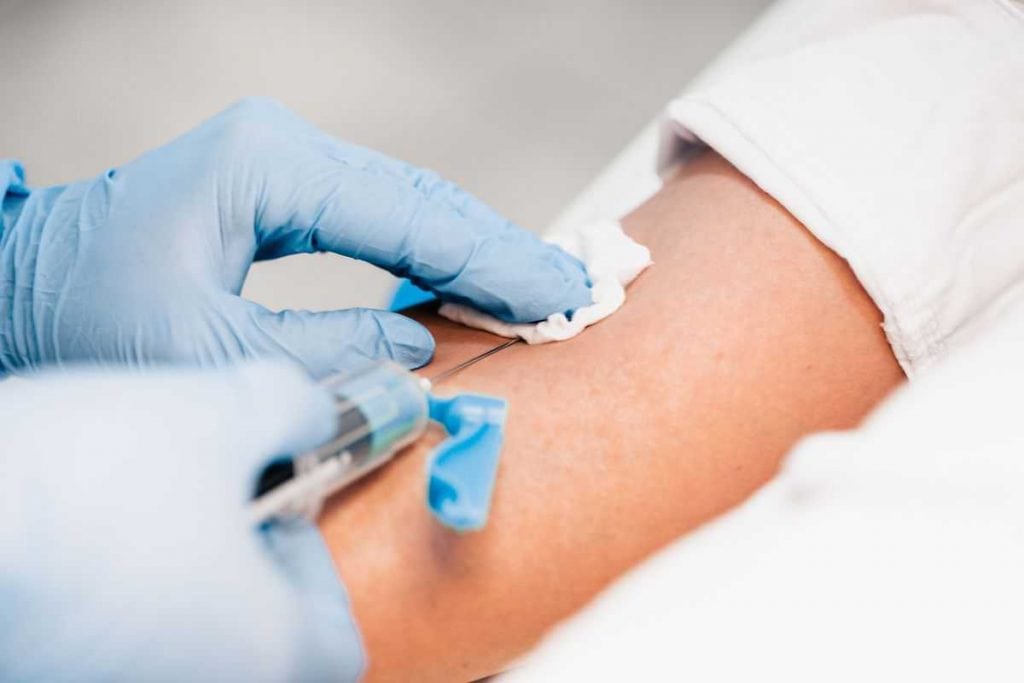
Extensive blood work will help doctors evaluate any risk factors you have that might increase your risk of pregnancy loss. Different doctors check for different items, but of special importance are thyroid tests and tests for antiphospholipid syndrome (APS). These tests check for blood clotting disorders and problems with your immune system that could lead to miscarriage.
Most doctors will also test your Anti-Mullerian Hormone (AMH) levels, a good indicator of ovarian reserve. (Meaning, do you have as many eggs left as someone your age is expected to have?)
One test that is becoming standard, but which many women still have to advocate for, is karyotype testing, which checks both partners’ chromosomal structures. If this test reveals a problem, you may be sent for genetic counseling.
Advocating for this test is especially important if you have a family history of recurrent loss, including not only your parents, grandparents, aunts, and uncles, but also your siblings (or your partner’s siblings).
*Note: Genetic abnormalities can run through any family line, so even if the person experiencing recurrent loss is your brother’s wife, it’s worth testing because you might carry a genetic translocation that you share with your brother.
Your doctor can also use blood tests, if performed at the proper times, to test for hormonal issues like progesterone production. Many researchers believe that low progesterone levels after ovulation can cause early loss, so some doctors prescribe progesterone supplementation beginning shortly after ovulation.
Anatomical Evaluation
Common causes of recurrent pregnancy loss include anatomical abnormalities (this was my problem, which you can read about here). The following procedures may be used to test for anatomical abnormalities:
- 3d ultrasound to look for uterine abnormalities (I never had one, but research suggests it’s common)
- Hysterosalpingogram (HSG) to check your fallopian tubes and uterus. For this procedure (which I have had), you will be positioned on your back, much like for your annual cervical exam. The doctor will insert dye into your cervix and watch via x-ray to see if it runs properly through your fallopian tubes and into your uterus. (This procedure is also common in infertility testing).
- Endometrial Biopsy to check the health of your uterus
- Hysteroscopy to check the health of your uterus and determine that there are no internal abnormalities, such as fibroids, septums, etc.
Less Common Recurrent Miscarriage Testing
Depending on your family history and physical health, there may be other tests doctors choose to run. If you describe certain problems in your medical history, you may be tested for Polycystic Ovary Syndrome (PCOS) or Endometriosis.
And I know there are more possible tests or conditions I am not aware of. I’ve heard women in groups I’m in discuss laproscopy for endometriosis. I’ve also heard talk of women receiving a lap and dye test, though my understanding (again, I’m not a medical doctor, so talk to yours) is that this is the more difficult alternative to an HSG.)
One final thing you can consider testing for is immunological issues (beyond those tested for in the original blood panel). Reproductive Immunology is a common practice in the UK, but less common in the US.
Many doctors believe in it; many do not.
One of the major practitioners in the US was Dr. Jeffrey Braverman, who recently passed away, but his New York-based clinic continues to work with Reproductive Immunology.
Another well-known US practitioner is Chicago-based Dr. Joanne Kwak-Kim Kahn.
Some Reproductive Endocrinologists are willing to consult with Reproductive Immunologists on your case. Others do not practice Reproductive Immunology at all and will require you to see a different doctor.
The Good News and The Bad About Recurrent Miscarriage Testing
Bad news first, always. 50% of RPL patients never find a cause for their losses.
But 65% of women who experience recurrent pregnancy loss can have a successful pregnancy with no intervention. So the odds are still in your favor!
Resources for Recurrent Pregnancy Loss Support
Need resources to help you through this journey?
Chat with other members of the Undefining Motherhood community to find people who understand your experience. Our Facebook page is a great place for this.
Reach out to Postpartum Support International for emotional support and help finding a therapist. Most postpartum mental health specialists are also trained in perinatal loss.
Online support groups. Keep in mind that online support groups are made up mostly of women who haven’t found answers and who are not medical professionals.
Still, they get you, and that’s huge. I cannot fathom having made it through my RPL experience without the support of women from the Facebook Group “Recurrent Miscarriage/Multiple Miscarriage Support.”
Tell me about your experience with recurrent miscarriage testing in the comments. What tests did I miss?
General FAQ
What causes recurrent miscarriage?
Recurrent pregnancy loss can be caused by a number of factors–blood clotting disorders, chromosomal abnormalities, poor egg or sperm quality, immunological disorders, anatomical abnormalities, and more.
Yes, most people consider recurrent miscarriage infertility. After all, the end result is the same–no baby.
Less than half of couples experiencing recurrent miscarriage find a cause, likely because science simply hasn’t caught up yet. There are more factors that go into the creation of a healthy pregnancy than we can possibly know, and testing will only improve over time.








7 thoughts on “Recurrent Miscarriage Testing: What You Need to Know”