When I had my first miscarriage at 8 weeks, I had no idea what to expect. We don’t talk about the physical process of miscarriage enough, or how different it is at different points in pregnancy and for each individual.
Since 1 in 4 pregnancies end in miscarriage, it’s absurd that women don’t know more about what to expect when miscarrying. So I’m here to tell you. Whether you’re experiencing an early chemical pregnancy or a late-term loss, a spontaneous loss or a missed miscarriage, here’s what you can expect of the process.
*Disclaimer: I am not a medical doctor; I have a

This site contains affiliate links, meaning that we earn a small commission for purchases made through our site. We only recommend products we personally use, love, or have thoroughly vetted.
What To Expect When Miscarrying
There are different types of miscarriage, so for the sake of simplicity, I’ll break them into 3 categories:
- Spontaneous–your body begins cramping and bleeding on its own
- Missed miscarriage–you find out at a doctors appointment, likely because of decreasing HCG levels (early miscarriage, before 6-7 weeks) or during ultrasound (later miscarriage, after 7-8 weeks).
- Ectopic pregnancy–an embryo implants in your fallopian tube instead of your uterus
This is, admittedly, an oversimplification, but it gives me a way to talk about the different possibilities. It also allows you to know where to scroll to, depending on what you’re experiencing.
I’ll talk about them in order.
One final thing you should know: the medical term for miscarriage is “abortion.” Be prepared, in case you see it on your chart.
1. Spontaneous Miscarriage

This will likely be listed on your medical chart as “spontaneous miscarriage” or “spontaneous abortion.” I’ve had 2 of these.
What Does It Mean?
You’re pregnant, and you begin bleeding and cramping. Heavy bleeding is often a sign of miscarriage in early pregnancy, although it can be caused by other problems, like a subchorionic hemorrhage (SCH).
Note: An SCH increases your risk of miscarriages, but about 50% of women who develop an SCH carry successful pregnancies.
What Will Happen?
You will start cramping and bleeding. For me, the two came at about the same time. Some people cramp first; others bleed first.
Now, when I say bleeding, here’s what I mean, and I’m going to get graphic because there’s no other way.
I mean bright red blood, and gobs of it. You’re soaking through pads. (Never put in a tampon during a miscarriage).
It’s not just runny red blood. It likely contains clots and clumps of fleshy pieces.
*Note: If you’re experiencing red spotting; contact your doctor. This could be an early sign of a miscarriage. It could also be a sign of something else, like a subchorionic hemorrhage (SCH). SCH blood can gush, but rarely contains clots.
If the blood is brown, it could again be an early sign of miscarriage. It could also be something as common as implantation bleeding. Believe it or not, bleeding in healthy pregnancies is not uncommon.
Miscarriage at 6 Weeks Gestation
When you ask what to expect when miscarrying at 6 weeks pregnant, most people will tell you it’s “like a heavy period.” This is sort of, kind of, a little bit true.
Yes, it’s like an extremely painful heavy period, but probably with a fleshiness to it. Cramps are generally much stronger than menstrual cramps, although some women do report period-like cramps.
More than likely, the bleeding and cramping will last a few days, with the most serious parts happening within a few hours.
Over-the-counter pain medicine will likely suffice to manage pain, unless you have an unusual experience (always possible) or a very low pain tolerance (no judgment here. I’m right there with you.)

For most women, an early miscarriage is not just a heavy period. It usually hurts worse, you bleed more, and there’s a lot more uncertainty.
Support people, please don’t compare this experience to a period and move on. That’s extremely unfair. Learn what not to say to someone who had a miscarriage.
When to go to the ER? If you soak through a menstrual pad in an hour, go to the emergency room. No one wants to risk passing out on their bathroom floor.
*NOTE: When I say pad, I mean a menstrual pad. Not a pantyliner or a small maxi pad. The big, thick things. I hate to say it, but I keep these on hand even though I don’t use them. Because if I ever get pregnant again and a miscarriage begins, I know this is my gauge. Go ahead and in the early weeks of pregnancy; you’ll need them postpartum anyway! The ones below are my favorite.
Miscarriage at 8 Weeks: What to Expect
At 8 weeks, you can expect a miscarriage to be bloodier, fleshier, and more painful than at 6 weeks. If you are open to pain medication, call your doctor, tell them what’s happening, and ask for a prescription.
Send someone to get it for you.
Do not drive.
You may be able to get away with over-the-counter meds, but honestly, I wouldn’t risk it. (This coming from someone who hates pain. If you can manage pain well, go for it!)
At 8 weeks, you’ll have cramps combined with a more minor version of contractions. Also, unless the fetus stopped growing earlier, you may see something that resembles a tadpole-like baby. Not everyone is prepared for this part, but it’s real. You’re birthing this tiny thing.
At this point, most women prefer to miscarry in the bathtub. It soothes the pain, provides a little comfort, makes cleanup easy, and you don’t need menstrual pads or heading pads.
But keep an eye on your bleeding and how you feel. Have someone vigilant around in case you start feeling lightheaded.
When to go to the ER? Again, If you soak through a menstrual pad in an hour, go to the emergency room. If you start feeling even a little lightheaded, go to the hospital, or call an ambulance if you’re alone. Do not risk passing out from blood loss in the bathtub!
Now, let me be clear, it’s not likely that you’ll pass out from blood loss. But it happens, which is why self-monitoring is so important. I never even came close. But I still know the signs to look for.
*Note: This advice is for the serious parts of miscarriage where you’re passing the baby. Bleeding and cramping can last for days or weeks, but there will be a more extreme time when you actually pass the fetus and gestational sac.
10+ Weeks Gestation
When miscarrying at 10 weeks, you can expect similarities to birthing at 8 weeks, but much more intense. You likely will have actual contractions. Not full on, 40-week labor contractions, but actual contractions. You have to give birth.
See all our notes about 8 weeks, and about bleeding at 6 weeks, but know that yours will be even more intense. At 12 weeks, it gets even more intense. 14 even more.
My recommendations for bathtubs and prescription pain meds get even stronger here.
And please don’t miscarry this late alone. If you’re alone, find someone to come over as support, or go to the hospital to be safe.
*Note: The timeframe of a spontaneous loss is extremely variable. My first natural loss lasted just over a week. I had 1 heavy night, thought the worst was over, until the next weekend when I actually, fully lost the pregnancy. But I cramped and bled in between–the in between was just like a period, but night 1 and weekend 2 were special beasts that in no way resembled my monthly menstrual cycle.
Second-Trimester Miscarriage
I have no experience here and would love for someone to write about it at some point. As such, I can’t tell you based on personal experience what to expect when miscarrying during the second trimester.
But my advice, based on people I know who’ve been through it, is to go to the hospital.
You’re giving birth. Your body goes through labor. Being medically supervised could be important.
2. Missed Miscarriage
What is a missed miscarriage?
With a missed miscarriage, you experience few to no symptoms. Everything seems to be going along fine.
Then, you go to the doctor, and you find out it’s not. This can be a real mindf***. I’m so sorry.
I am so, SO sorry.
With a missed miscarriage, you’re simultaneously in the best and worst of situations, given the circumstances in terms of what to expect when you miscarry.
It’s the best of situations because you get to choose how to proceed.
It’s the worst because you have to choose how to proceed.
Here are your choices.
Option 1: Dilation and Curettage (D&C)
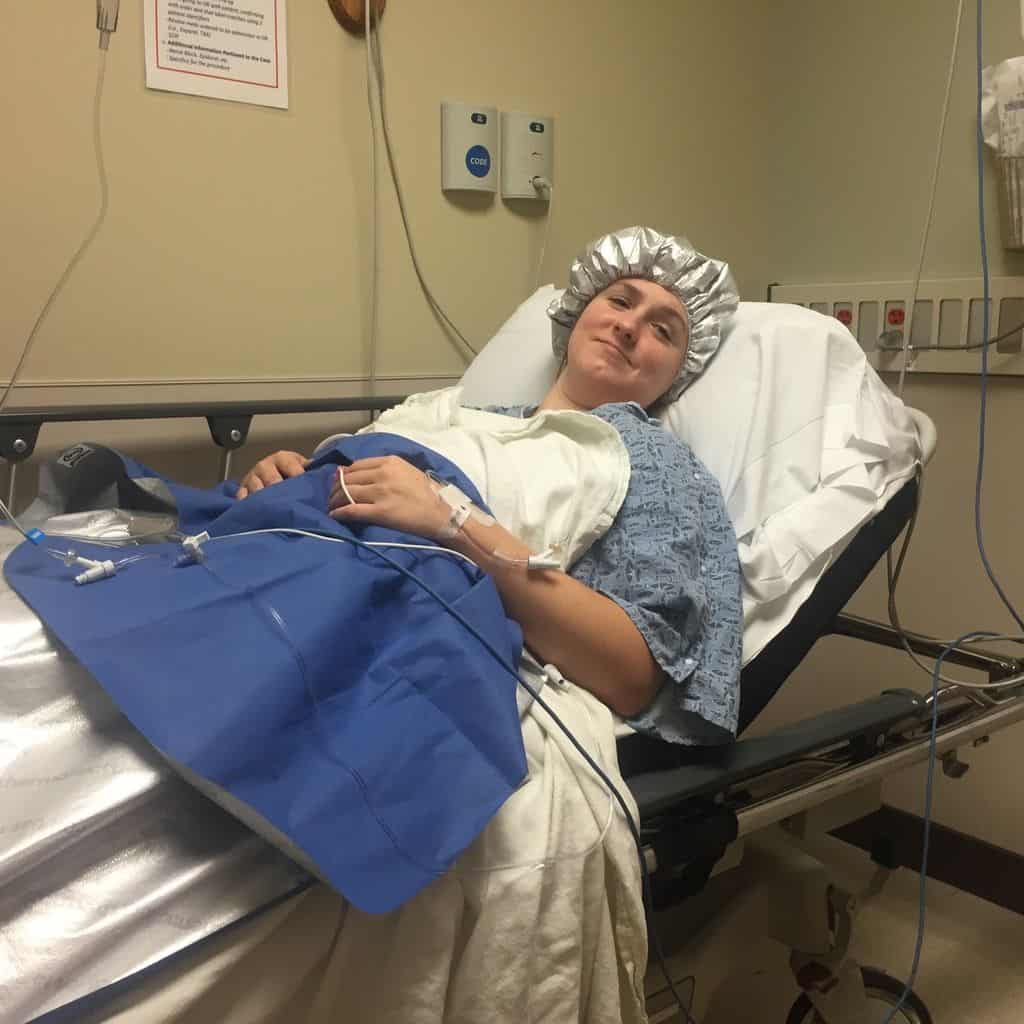
A Dilation and Curettage (D&C) is a surgery in which your doctor will clean out the contents of your uterus.
I’ve had 1 of these.
What should you expect if you choose a D&C when you’re miscarrying? You schedule surgery, go in, come out, and recover. It’s a minor surgery with a minor recovery. At least physically. The emotional toll will vary greatly. If you’re in the US, it’s costly.
Talk to your doctor about the risks, pros, and cons, to help make this decision. Here are a few:
D&C Pros:
Control. This whole experience feels so out of control, but if you choose a D&C, you schedule the time, the place, and the doctor. You know what to expect.
Anesthesia. You’re put to sleep (if a doctor ever says they’ll do an epidural, please, probe as to why they aren’t fully anesthetizing you). You’ll wake up, and it’s over. Physically, at least. You may cramp and bleed for the next week or so, but minimally. Physically, I found this to be MUCH easier than natural losses.
D&C Cons
Anesthesia again. Being anesthetized is really scary for some people and certainly comes with inherent risks.
A medical experience over an emotional one. This method is extremely medical–if you need the closure of birthing and seeing whatever has grown of the little one you’ve been carrying, a D&C probably isn’t for you.
Scar tissue build-up (Asherman’s Syndrome). There is a very small risk of scar tissue buildup that can cause problems later, especially if you have multiple D&Cs. The risk is low, but if it happens, it can cause complications in later pregnancies, as well as with your menstrual cycle.
Cost: If you’re in the US, this procedure can be very expensive. Talk to your hospital about cost before moving forward with the procedure.
Option 2: Wait to Miscarry Naturally
If you make this choice for your missed miscarriage, go back to our discussion of #1: Spontaneous Pregnancy Loss, to learn more about what to expect.
My doctor strongly discouraged this option because my body was showing no signs of miscarrying on its own.
My HCG levels were rising, I was not cramping, not even spotting.
If you’ve been cramping and mildly spotting, or if your hormone levels are dropping, it might happen sooner for you.
Natural Loss Pros:
Confidence. You feel 100% confident that you did the right thing. I never questioned whether my diagnoses could’ve been wrong, but some women do. If you aren’t 100% certain that your pregnancy is over, waiting is essential.
Knowing Your Body Can Do This. Losing a pregnancy makes many women feel like their bodies have failed. A natural loss can often serve as an emotional reminder that your body is handling reproductivity on its own.
Natural Loss Cons:
Risk of infection or other complications. If your body carries a non-viable pregnancy for too long, you risk developing very serious infections and other potential problems. Talk to your doctor about those risks. So, if you’re showing no sign of miscarrying naturally, it might be risky to wait it out.
Option 3: Medically-Induced Miscarriage
This means you take a medication like Misoprostol/Cytotec.
Your doctor may tell you to take it orally or may instruct you to insert it vaginally.
I have seen abundantly varying results with this option, which is why I have never chosen it. It’s also the hardest to tell you what to expect because it is so different for everyone.
(This is true of all types of losses and interventions, but especially of medically-induced miscarriage.)
For many women, it works beautifully and they miscarry quickly. In these cases, refer back to #1: Spontaneous Pregnancy Loss. Note that many do report experiencing heavier cramping with Misoprostol than with spontaneous losses.
For other women, however, this medication causes extreme pain, excess bleeding, and/or doesn’t lead to a full miscarriage, meaning they still end up needing a D&C. However, I don’t have statistics on this.
I have never chosen this route because I’m admittedly afraid of it. I know tons of people who thought it was an easy drug to take, but I know many others who experienced major complications with it.
If you choose this route, my suggestion would be to ask for prescription pain medicine in case you need it and to never take it alone. If you’re among the women who experiences complications, you’ll need a support person within quick ear’s reach.
Medicated Pros:
Choice/timing. You can choose the time you take it on your own terms, but be able to experience the actual loss at home. It’s a good in between option between waiting for a fully natural loss and having a D&C.
Cost. If the choice is medicated induction vs. D&C, you come out spending WAY less money with medication.
Medicated Cons:
Partial miscarriage. If the medication does not cause a complete loss, you may still end up needing a D&C.
Complications. Some women report excess pain and bleeding.
Social Judgment. When you read stories about about pharmacists refusing to give out “abortion pills,” this is what you’re reading about. I don’t personally know anyone who has experienced this, but I’m terrified of how hurtful it would be.
Anecdotal evidence makes it seem like a larger number, likely because people who had bad experiences are more vocal. Thus, while I’m most hesitant about this option, research does not indicate that I actually should be.
3. Ectopic Pregnancy
This is a completely different scenario than any listed above, and it’s honestly much more serious. I have had 1 of these.
What to expect with this an ectopic pregnancy depends on how far along you are in your pregnancy. Look for the signs early, especially if you have a history of ectopic pregnancy. If you’re interested in ectopic pregnancy stories, you can read Beth’s here.
If you experience any signs of an ectopic pregnancy, please see your doctor immediately.
- Extreme pain on one side of your abdomen. I don’t mean cramping; I mean a sharp, stabbing pain that comes and goes intermittently.
- Plateaued HCG levels. If your doctor is monitoring your HCG levels and they plateau, request an ultrasound immediately. Even if you’re so early they say they won’t be able to see anything, ask for a “placement scan.” Do they see anything in your uterus? Do they see anything in either of your fallopian tubes?
Please be vigilant of the signs of ectopic pregnancy. In the worst-case scenario, your fallopian tube can actually rupture, which can cause your body to become septic. This is a life-threatening condition.
If an ectopic pregnancy is confirmed (or suspected while a nonviable pregnancy is confirmed), you have 2 options (that I know of), but less choice than with a missed miscarriage. It largely depends on how far along you are.
Ectopic Pregnancy Option 1: Methotrexate Injection
Methotrexate is an icky but important drug used to treat some types of cancers, psoriasis, and rheumatoid arthritis. It’s also extremely useful in the treatment of early ectopic pregnancy because.
I know this sounds so weird and terrible, it literally dissolves the contents of the pregnancy.
There are a lot of cons to methotrexate in terms of side effects, so talk to your doctor about it.
But here’s what I will say. If your ectopic pregnancy is discovered early enough, this drug can be tube-saving and life-saving.
But here’s the thing–those contents, products of conception, fetus, baby, whatever word you’re most comfortable using–is growing in your fallopian tube!
There is zero chance of its survival, and not taking care of the situation could cause you to lose your fallopian tube. It could even lead to maternal death.
Physically, this was my “easiest” loss. I went to the ER one night, had a confirmation scan, and was given a shot. I didn’t bleed, and I didn’t cramp. Physically (not emotionally), it was as if I’d never been pregnant at all.
Ectopic Pregnancy Option 2: Surgery
I’ve never experienced had surgery for an ectopic pregnancy, so I can’t speak personally about what to expect.
But if your ectopic pregnancy is discovered too late for methotrexate to be an option, your doctor may need to perform a surgical procedure to remove all the contents from your fallopian tube.
To read more about the experience of this surgery, check out Beth’s ectopic pregnancy story.
It’s possible they’ll need to remove the fallopian tube.
(If you lose 1 tube but have another, you can still get pregnant naturally, but we all know this is no one’s ideal scenario).
Summary
Pregnancy loss sucks, and it’s different for everyone. I hope this rundown helps you understand what to expect your body to go through when you miscarry. I hope it can help those around you understand the same thing.
Your stories can really help others going through miscarriage understand what to expect. I’m especially curious to hear from those of you who have taken Misoprostol/Cytotec or who required surgery for an ectopic pregnancy, since I can’t speak to either of those personally. Let’s all be open about our miscarriage experiences to help each other during tough times like these.

What was miscarriage like for you? Share your story in the comments!
General FAQ: What To Expect When Miscarrying
When should I go to the emergency room for miscarriage?
Go straight to the ER if you soak through a menstrual pad in an hour, or if you start feeling lightheaded.
It’s not always obvious. If you start bleeding bright red blood and cramping simultaneously, it’s likely you’re miscarrying.
Bright red bleeding or spotting without cramps could indicate miscarriage or a subchorionic hemorrhage (SCH). Contact your doctor if you’re concerned.
It’s different for everyone. The major part of the miscarriage will usually happen within a day, but bleeding and cramping can last days or even weeks.
Early, it feels like heavy cramping, generally stronger than period cramps. Further along, you have actual labor contractions, although the intensity varies. In those situations, your stomach tightens (and cramps, but tightness is a better indicator), usually in varied intervals.
It is possible to miscarry and then retain tissue in your uterus. This is called an incomplete miscarriage, and it can lead to complications if not treated quickly. You’ll likely have to take Cytotec (misoprostol) or undergo another D&C to clean out the remaining contents of your uterus.
Pregnancy testing at home will continue to show positive tests as your human chorionic gonadotropin (HCG) levels decrease. Having your doctor follow your blood levels down to zero can be a good idea.
More Miscarriage Articles
- Coping with miscarriage grief
- Creating miscarriage memorials
- Recurrent miscarriage testing checklist
- Why you don’t have to attend a baby shower after miscarriage
- After miscarriage, what to do
- Books about miscarriage
- Reader-favorite miscarriage tattoos
Miscarriage Stories
- Katy’s success after recurrent miscarriage
- Beth’s ectopic pregnancy story
- Arden’s misoprostol experience
- Katy’s blighted ovum story










December 2015/January 2016, I endured what was an (initially missed) ectopic pregnancy. I unexpectedly learned I was pregnant on December 18th and began bleeding the 21st. By the 23rd, I was diagnosed with a miscarriage via two quantitative HCG tests and sent home to ride it out.
By late Christmas Eve, I was in horrific pain, and my husband rushed me to urgent care, who immediately sent us to the ER. Another quantitative HCG was ran, and this showed a small spike after the previous decline.
IF YOU HAVE THIS HAPPEN, REFUSE DISCHARGE UNTIL A PLACEMENT SCAN IS DONE.
My normal OBGYN (who was on vacation when this all started) later informed me that a spike after a decrease can signal ectopic pregnancies, but the ER we rushed to chose to not perform an ultrasound and ignored my requests, telling me I was hysterical. As a result, the on-call midwife listened to the ER over me. I suffered until January 8th with that ectopic pregnancy. By the time my doctor found it, the mass was the size of a ping pong ball and had partially ruptured my left tube. I had surgery that afternoon to remove the tube.
Though the surgery physicially was one of my easier recoveries, mentally it was traumatizing. Even though I went on to have a healthy child later that year, I spent the entire pregnancy in fear and still fear another one.
Thank you so much for sharing! I’m so glad you mention the minor spike in HCG levels! I mentioned plateaus, but not spikes. Such important info. We have to know a lot and advocate for ourselves and our bodies so much!
I’ve experienced early, late, missed, spontaneous, d&c and blighted ovum pregnancy loss, I often talk about it on Facebook and Instagram when I had a public account. I am always open to discussions because so many people think all miscarriages are the same. A bad period and that’s it. It’s not. I’ve ended up in the ER twice and I needed emergency surgery for one of them. I felt my water break during contractions and I saw my son come out. He had eyes, ears, a nose, arms, legs, fingers, toes, and his little mouth was wide open. No one asked me if I was ok after it happened, everyone pretends nothing happened because it’s easier for them. So I speak about my experiences for those like me, you’re not alone.
Thank you so much for sharing this story! It’s horrible and makes my heart ache for you, but it’s also what people need to hear!
I wish I was able to find a resource like this when I was miscarrying. Instead, I asked my midwives a thousand questions only to get partial answers, because they didn’t want to commit to telling me what it would (or might) be like.
I miscarried after discovering I was pregnant with an IUD in place. The IUD was removed, and I began bleeding that night. I was estimated to be about 5 weeks along. Maybe because I was so early on, but mine was thankfully very light, and less painful than some periods, but there was still slightly more clotting (though again, this was minimal). For me, one of the hardest part was reconciling the fact that I was 1) pregnant despite having an IUD in place, and 2) already feeling conflicted about having another child. In a lot of ways it made me want another more. This was 2 months ago, and I still havent really come to terms with this aspect of the loss.
Thanks again for sharing this informative post.
It’s so tricky emotionally! I just don’t understand why no one wants to be honest about what you should expect. It’s so frustrating.
Thanks for sharing your story. I’d like to add my own to your description of ectopic pregnancy. I had an ectopic pregnancy rupture at 6 weeks. Most doctors don’t want to do an ultrasound until 7-8 weeks, so it’s important to know that the pain from a rupture can present in many different ways. Sharp stabbing pain on one side, yes, but it can also present as a more amorphous abdominal pain or even a displaced pain in the shoulder. When I had mine, it felt like gastric distress. I thought I had food poisoning at first. I had never been pregnant before, so part of me wondered if this was some kind of morning sickness. The pregnancy book I had described ectopic pain only as shoulder pain, so I dismissed that. If you feel any sort of weird pain, get it checked out ASAP. I quickly found myself fainting and in shock. When I got to the hospital I had to have emergency surgery and a transfusion.
We lost our child at 15 weeks and 2 days. In hindsight I should have known the cramping all day was contractions. They were small at first but didn’t last long and came in waves. But all day I was in deep nesting mode. Deep cleaning things that were not necessary.
By bed time the cramps were intensifying. Creeping around from my abdomen to my lower back. My husband fell asleep quickly and soundly as I writhed in pain beside him in our bed. And then it happened. I don’t know how to explain it other than there was a “twinge” like something broke. Maybe it was supposed to be my water (I never experienced that in my first pregnancy), but there wasn’t an immediate gush of anything. At first it was a slow trickle of dark brown blood.
I immediately called my OB office after hours line as it was around midnight at this point. I was starting to pass slightly more blood and it was starting to get lighter in color. The doctor returned my call and said if it was a significant amount of blood I needed to get to a hospital, but I didn’t make it. I sat on the toilet in our home and fully delivered our child. It happened just that fast. At this point I began hemorrhaging blood.
I yelled and beat on the walls until my husband awoke. He came around the corner to me hysterical and bleeding uncontrollably and our child already here but connected by a shriveled umbilical cord.
The next moments are a blur. Waking our 3 year old daughter and getting her in the car. Putting on layers upon layer of clothes and towels so I didn’t bleed through everything (I still did). Getting her to grandmas as quickly as possible.
We were leaving their house destined for the hospital my OB was located but I was bleeding so heavily and in so much pain (still having contractions) that I told him to go to the nearest hospital. They were supposed to be really great for delivering as well.
I laid in the ER for 8 hours before an OB arrived for the day. Eight hours of contractions and hemorrhaging. Of pain both emotional and medical. The ER doctor tried his best but was in over his head. My BP dropped very low and they were extremely close to giving me a transfusion (I don’t remember much there as I was going out of consciousness).
We called my mom around 6 am and she drove an hour to be there. I had the DNC around 8. I spent the next week in our dark living room recovering. The first 2 weeks I had a migraine so bad I could move my head and my shoulders slumped.
We got past it all though, one day at a time. I lost that entire month in mourning. But here we are, currently 16 weeks and 4 days into our next pregnancy. I am still terrified everyday. Every time I go to pee I can feel the rush of everything coming out all at once again. I have been set to high risk and we are doing extra ultrasounds, but those feelings never escape you.
Thank you so much for sharing, Lindsey! What a horrific experience. I am so, so sorry. Pregnancy after loss is so hard; and pregnancy after such a traumatic loss is nearly unimaginable. After 4 losses, I had Jack, who is now 19 months old, and I STILL check toilet paper every time I wipe. It’s amazing how these things become engrained in you. I have a post about pregnancy after loss that might give some helpful tips if you haven’t read it. Ultimately, though, it’s one day of fear and hope at a time now. Please keep me posted on this pregnancy! All the best to you, mama.
I’ve had 3 pregnancy losses. The first was a blighted ovum – my doctor gave me the option of waiting for it to occur naturally (which I knew from friend it doesn’t always happen and could result in a D&C) or cytotec – I chose the cytotec as we had a fishing trip planned with friends and didn’t want to have complications with a miscarriage in the middle of Lake Michigan. Cytotec is horrible (but at least you can choose when the loss will happen). 2 nights in a row inserting 5 pills vaginally. I didn’t have a lot of bleeding – just horrific pain that the prescribed pain meds didn’t even touch. My hubby was great though – ran a hot bath at 2:30am. The miscarriage is supposed to happen within 48 hrs of the first dose….I didn’t miscarry until the 3rd day.
My 1st tubal – I had NO pain – barely mild cramping. I started bleeding – called my doctor – told to just monitor it as in had an appt for a 7 week ultrasound in 4 days (infertility treatments – 7 week ultrasound part of routine to confirm pregnancy and release you to your regular OB). They were in shock I wasn’t in pain (mind you I have a HIGH pain tolerance). They sent me for bloodwork – “prepped” me for surgery (was told no eating or drinking) – and told me to go home and wait for them to call with their decision of surgery or methatrexate. They called and told me to head to the hospital’s infusion center for methatrexate. I had light bleeding with this 2-3 weeks. Then they had to do a HSG to make sure it completely cleared out – which the cramping after that is NOT fun!!
My 2nd tubal – again infertility treatments – I tested negative for pregnancy 2 weeks after treatment. Started cramping (to me mild cramps but remember HIGH pain tolerance) and was cramping for 3 days – waiting for my period to start but never did. The 4th day of cramping was 3 weeks post treatment – took another pregnancy test and it was positive. I went to work – on my way cramping got worse and felt like I had heartburn (NEVER had heartburn before – not even while pregnant). Once at work had a sharp shooting pain that almost made me faint and hot flashes. Called my doctor – they told me to go to the ER to get checked. So I did….after work – as pain kind of subsided – go to the ER. They did an ultrasound – found I had an ectopic pregnancy that ruptured and had blood starting to pool in my lower abdomen. I still hadn’t taken any pain meds – which amazes the ER staff and my doctor when she got there. Went in for emergency surgery – even walked into the OR. Recovery physically wasn’t too bad – 1 week off work. What was hard was the mental and emotional recovery – especially difficult that 1st week as my 2 yr old couldn’t understand why mommy couldn’t pick her up and carry her. Hard emotionally as I have 3 scars that are daily reminders that I lost a baby (and a tube). Hard emotionally as I really want another baby but scared I’ll end up with another ectopic and lose my other tube and not be able to have another baby. Hard emotionally as my husband wants another baby but is scared shitless of another ectopic pregnancy and potentially losing his wife as I have a high pain tolerance so I unfortunately don’t take things as seriously as I should
That being said – and still dealing with the emotional rollercoaster daily – we are gearing up for another round of infertility treatments. Finger crossed things go in our favor this time. My doctors will have no under high survailance this time around – they aren’t taking any chances.
I’m so glad they’ll be monitoring you so closely this time! I’d love to hear more from you about the types of testing you’ve had done. I imagine they’ve run the gamut, but I have a unique experience with this, so I like to know what people have done and make sure they’re fully covered. And yes–HSGs SUCK!!!!! I couldn’t believe how much cramping I had after my HSG or Endometrial Biopsy. So much more cramping than I expected.
I’ve had three miscarriages and have one child (and another on the way!). I got a d&c after my first miscarriage. I woke up from the anesthesia sobbing like I’d had my baby ripped from me (I guess I technically did) and had a bad reaction to the medication they gave me. All of my muscles were so sore that I could barely move for a couple days. I passed my second and third babies naturally but even those were SO different. With my second baby, I was about 10 weeks along when the miscarriage started but we had known for a couple weeks that the baby died. She measured about 6 weeks in size. Bleeding started in the evening and I got contractions the next morning. They were more intense and painful than the contractions I had when I gave birth to my full-term son! I didn’t know what was happening since my doctor told me I’d have a “heavy period.” After about 45 minutes of intense pain I was sitting on the toilet and a nerf football sized object shot out of me. It was like the entire thing came out all at once. The relief I felt was instant and the pain was gone. I had barely any bleeding after that, too. I was able to bring it to my doctor and they did testing to find out what went wrong. With my third miscarriage I started spotting at about 6 weeks before I knew anything was wrong, and by the time I got an ultrasound they couldn’t find the baby anywhere. We were concerned about the possibility of an early ectopic pregnancy but eventually that got ruled out. That miscarriage felt much more like a “heavy period” and I didn’t pass a lot of tissue like I was expecting.
This is a great reminder of how different each miscarriage is! It’s hard to account for that in a post about “what to expect” because no one wants to hear that it’s always different. But it is always different, and what I’ve outlined is a guide, not a given. I really appreciate you sharing these experience. And congratulations on the 1 you have and 1 on the way!
In April 2017, I discovered I was pregnant unexpectedly. I was on birth control at the time and didn’t have a regular period so I wasn’t really sure how far along I was but assumed only a few weeks. Went to the doctor, she scheduled an ultrasound for 2 weeks down the road to “date” the pregnancy and go from there. As I said, it was unplanned and unexpected but we quickly became excited about having a baby!
Fast forward to my ultrasound on a Friday afternoon – I’m the last appointment of the day. Again, we’re assuming I’m not that far along and the ultrasound tech automatically goes for the transvaginal approach asking me to urinate first. She then decides that I’m probably further along than we thought and should have gone for a traditional abdominal ultrasound. But she needs my bladder to be full. So she has me get dressed and go to the waiting room and basically chug as much water as possible for a half hour or so. At this point the imaging center is basically empty – she tells the janitor that we’re gonna be a little late and not to lock us in.
Back to the room now. Cold gel. Search search search. Hold on. Meanwhile, I see the look on her face. Again, I’m not in the doctors office but a medical imaging center. Everyone has gone home for the weekend. I’m starting to get freaked out. Eventually she tells me that she’s not supposed to say things like this….but she doesn’t know what to do. My doctor is out of town at a conference for the weekend. The office is closed. No other doctors around. It’s Friday afternoon and everyone is gone. She left a message and someone is should call me. But “something is wrong”. She was incredibly apologetic. I didn’t know what to do. Tried not to panic. Waited for my phone to ring…but nobody called.
NOBODY called me all weekend. I just waited and waited and waited for my phone to ring. Tried to stay sane. Sunday afternoon I started “spotting” and called. Got the answering service obviously, told her what was going on and she actually told me that some bleeding was nothing to worry about and that my doctor was still out of town but she’d pass the message along to her. She just brushed me off.
Sunday night/Monday morning I had a terrible time sleeping. Started cramping. I didn’t want to believe what I knew was happening. Just tried to tell myself not to jump to conclusions until I heard from my doctors office. Tried to tell myself that maybe nobody called because the ultrasound tech was wrong. I was going to the bathroom every 10 minutes. Most intense “cramps” I had ever experienced. I actually got up and started getting ready for work. With tears in my eyes because the cramps were so bad. My s/o kept telling me to stay home but I just wanted “normal” so I kept trying to get ready for work. Hobbled to the basement for some clean work pants out of the dryer when I felt a sudden gush of blood. And I just screamed and cried. Ran to the bathroom sobbing. Yelled at my s/o to leave me alone. And I sat on the toilet and miscarried what I eventually found out was my 15week old baby. It all happened really fast….or it felt fast anyway.
So I called off work went to the Emergency room where they did an ultrasound to be sure it was a complete miscarriage. Got the whole “sorry for your loss here’s a maxi pad” speech and they sent me home. Told me to grab something over the counter for pain and that they’d call my doctor.
So there I am, driving myself home. Crying. And my doctors office calls me. It’s a nurse, my doctor isn’t in yet but they got a message from the imaging center on Friday and want to schedule me to come in. I informed her that they were too late, I had a miscarriage and had just left the ER. I’m pretty sure I was rather rude to her before I hung up but I told her I was already halfway home and wasn’t turning around to come into the office today. I went home and slept. My actual doctor finally called me on Tuesday to apologize.
It was absolutely awful….but I’m so thankful for that ultrasound tech who was honest with me. I never told anyone from my doctors office or the hospital that she had warned me something was wrong because I didn’t want her to get into trouble but I’m grateful. Had she just sent me on my way that afternoon with a made up excuse I never would have known the difference and would have been completely blindsided by the miscarriage.
Fast forward to now, almost 2 years later, and I’m 23 weeks pregnant with a little girl. And I have a new OB this time around (disclaimer: my previous OB wasn’t very nice but after the way everything was handled I couldn’t go back there) who I LOVE. I still have anxiety that something is going to go wrong – especially when I go for an ultrasound. However, so far everything seems to be fine.
I still find comfort in reading other people’s stories about pregnancy loss – glad that we have eahother and forums like this to share our stories.
Thank you so much for sharing! Your story makes my blood boil. I had a similar confusing and awful ultrasound experience with my first loss, except the ultrasound tech lied to me, told me I was likely earlier than I thought, then lied to my doctor and said she’d adequately warned me, so the doctor didn’t think she needed to call. Even with Jack, I feel panic when I walk past that ultrasound room. I’m so thankful you have a new doctor and new pregnancy! 23 weeks is huge! I never relaxed, but 24 weeks definitely made me feel better.
I had a D&C, it was a really hard choice but for me I felt seeing him and doing it alone would be more traumatizing.
It is a mindf*ck though because I was in school denial after the procedure, I remember waking up believing the doctor was going to tell me ‘sorry our bad, you’re still pregnant’
There is no right or wrong way to miscarry you just have to follow your gut and do what you believe is best for you.
Good read.
Yes! I’m so glad you made this point! It’s so hard to write about this subject without apparent bias. I know what was best for me, but it is NOT what’s best for everyone. It’s such an intense and individual decision. Thank you for sharing!
After six years of trying I took a pregnancy test on a whim and got the surprise of my life…it was positive. It was the day before April Fool’s day so I was afraid to share with anyone besides my husband but I did end up telling my mother. We had a wonderful week of knowing we were finally pregnant and would finally be able to grow our family. I had had some light spotting that was all brown or pinkish and didn’t worry too much. But eight days later the blood became bright red and miscusy. We got into the OB the next morning and while she didn’t see anything on the ultrasound she initially thought it may just be too early. But a physical exam revealed an open cervix and she thought she saw tissue trying to pass. I felt my baby pass from my uterus as we were walking to the car. I sobbed so hard I nearly threw up. 10 weeks later I was in the ER after a week of pain and feeling increasingly bad. Blood work showed we were pregnant again and an ultrasound sound shows a heartbeat and a baby nearly seven weeks along. I gave birth to a daughter via emergency c-section four days after Christmas. I had a hard time enjoying my pregnancy as I was in fear of losing her for most of it. I am still struggling to come to grips with the sudden end of this pregnancy even though it resulted in a live birth and healthy child.
September 2018 I had a miscarriage at 6+5 weeks. What started out as light bleeding ended up being 5 torturous weeks of heavy, painful bleeding. Around two and a half weeks of bleeding my doctor said I wasn’t eligible for a d&c anymore because my ultrasound showed that I had passedmy little bean already therefore I had to wait it out. Three more weeks go back and she finally decides to prescribe me misoprostol. Now I was very hesitant to take it but the physical and emotional daily reminder had taken a huge toll on me and I couldn’t do it anymore. So I took it and i was extremely uncomfortable, I didn’t go to work for the next two days because of how much I was cramping and bleeding but it was because my uterus was contracting more because of the meds and therefore pushing out the remaining lining that’s was keeping my HCG levels elevated. The pills helped complete my miscarriage within two days and I was very grateful for it.
I had two miscarriages. My first was a blighted ovum. My second I had a DNC, unfortunately this caused Ashermans syndrome. I wish I had known more about Ashermans sydrome, but I was so sick and couldn’t stop throwing up for no reason. My levels were rising, no heartbeat. Doctors were concerned about a molar pregnancy. After a surgery I was able to conceive our daughter but have had many issues related to the Ashermans since so we adopted our last two. I wouldn’t change our family. I wish they would explain the risks more fully. I don’t know if it would have changed anything. Ashermans is horrible!
I so appreciate you sharing this experience, Sarah! I know Asherman’s is rare, but terrible, and it’s not something I can speak to. I think hearing those stories is so important because it is part of being educated about a D&C. I’m so sorry for your experience, but I’m glad you have the family you love, and I appreciate you being open with us here!
I’ve had the trifecta of first trimester miscarriages. A blighted ovum at 8 weeks that was medically miscarried, a d&c at 10 weeks (after the meds didn’t work) and a spontaneous miscarriage at 6-7 weeks.
What I liked about the meds was I could do it at home and it was like a mini-labor. It brought me a closure that was helpful, sort of way of saying goodbye. They start to loose effectiveness in the 9th week esp if the fetus/baby has gotten too big. However I will be frank and say the only time I’ve been in worse pain was when I gave birth.
I switched GYNs and my new one does not like her patients to take them vaginally l. They did not work when I took them orally, The meds did work when I took them vaginally with the first pregnancy, but that was also a blighted ovum. She did give me permission to try again vaginally, but by that time my toddler and husband was sick and I decided to just go for the D&C.
The spontaneous loss was the hardest emotionally. In my mind I’m prepared now not to hear that heartbeat at the ultrasound now, but the sob that came out of me when I saw the blood was….animalistic. I bled during my daughters pregnancy too..but this time I knew it was different.
Thank you for sharing. It’s a terrible club we’re in, but it’s good to know we’re not alone.
It’s such a terrible club! I’m sorry you’re a part of it, but glad to meet another member. Thank you so much for sharing your experience! I know it will help people who find this page trying to decide between Cytotec and D&C. Much love to you, mama ????
My dear cousin, Sarah Creel, PhD, sent me your blog information this week. This is the first post I’ve read and I am so glad I did.
We found out I was pregnant 12.31.18. This was my first pregnancy, we were trying to get pregnant, and we were beyond thrilled!
We had our first ultrasound on 1.23.19 (at about 6.5 weeks along) and saw our precious baby’s heartbeat. Everything checked out and we scheduled the next appointment for 2.21.19 (10.5 weeks).
During the 4 weeks between appointments, I experienced all the things pregnant women experience. To me, everything seemed completely normal.
On 2.20.19 I noticed some blood on the tissue when I used the restroom. I tried not to panic. I immediately called my OB who had me come in to see him. My husband met me there. We waited for what felt like the longest 15 minutes of my life. He took us in the exam room and he could not find a heartbeat on the doppler (which he should have been able to see at 10 weeks and 4 days). We then immediately went to have an ultrasound. The sweet ultrasound technician quietly stated, “there’s no heartbeat.” To say we were devastated is an understatement. The technician said the baby measured around 6-7 weeks along, which means it passed away shortly after our first ultrasound.
I’ve unfortunately have several friends who have experienced miscarriages, all at different stages in pregnancy. As a result, I was instantly worried about a miscarriage when I found out I was pregnant. Sadly, we did experience it.
We chose to have a D&C done since I was at 10.5 weeks along and the miscarriage had not occurred. I honestly didn’t want to wait. The D&C itself was quick. However, I had a good bit of pain and bleeding after. My doctor told me I would need to take Cytotec twice daily and doxycycline twice daily. He said the Cytotec was to help contract my uterus to expel anthying remaining and to help it return to its normal size. The doxycycline was to prevent infection. He also gave me heavy duty pain medication, which I took for two days. I’m 4 days out from the procedure and finally feeling better, the cramping is still there but much less intense. I took off 4 days total from work and returned today.
I’m becoming more emotional with each day. I think it’s all sinking in and becoming a reality. It’s difficult to remember that I’m not pregnant, if that makes any sense. I’m also anxious about the days ahead and our next attempt to get pregnant. What am I going to do if it happens again? That anxiety weighs heavily on me. Lastly, I worry about my husband and hope that he’s handling things okay. He’s been so supportive of me in every way, but I want to be sure he’s grieving as he needs to and that he has the support he needs.
I apologize for the extra long post. I hope that this helps someone else with their journey.
Thank you so much for sharing, and I’m so sorry for what you’re going through. I have numerous posts about this subject under the Pregnancy Loss category, and am working on getting a post from the male perspective. Please reach out if you need to vent. It’s such a hard experience that I know far too well!
I went in for my 8 week appointment (ultrasound) and was told the baby was measuring smaller than they expected. I got blood work done that day and was told to go home and come back in 2 days for repeat blood draw. Long story short my hcg level was dropping and I was having a missed miscarriage. I was prescribed to insert the pills vaginally and basically “wait it out.” I stared at them on the counter for a long time, it’s hard taking an action that you know will end in something heart breaking. A lot of the advice I had received was just wear sweats, find a place on the couch, and just settle in. I did that for awhile but I have trouble sitting still in general (there’s laundry to do or dishes to be put away), after a few hours I took our dog for a walk and survived the day so to speak. After 30 days I hadn’t gotten “a normal period” so my doctor recommended taking an at home pregnancy test, and let me tell you how traumatizing it is to take a pregnancy test and hope it’s negative. Well mine was still positive, so I had to take the pills again, this time orally. Then after another 30 days I had a negative test. A miscarriage doesn’t always just happen in one day, mine took 2 and a half months. The pills alone weren’t terrible it’s more the emotional toll they took. I do have factor IV (a blood clotting disorder) and that “could” have been the reason but it’s hard never knowing. Trying again now and every month I put so much pressure on myself….
I totally hear you on the pressure, and I’m so glad you pointed out.
Have you been told to take baby aspirin next time? If not, definitely ask your doc. I’m so sorry for your experience, and that it took so long!
❤️❤️❤️
I experienced four losses. It is very painful, emotionally. A lot of people do not understand. We had three losses after our first child and one after our second, before our third. My first loss was between 8-10 weeks, spontaneous, I was at home. The whole process from cramping to delivery was about one week. I delivered the baby at home, it was intact as well as the sac, and you could clearly see all of its tiny features. The second was a missed miscarriage. I went in for an ultrasound between 7-8 week and there was no heartbeat. I was scheduled for a D & C after bloodwork came back to confirm a non viable pregnancy. The third was spontaneous, very eary pregnancy. I had an appt at the first part of the week and confirmed pregnancy and miscarried at home by the weekend. The fourth loss was at 19 weeks. I had a significant amount of blood loss and I went to the ER, they called it fetal demise. We were scheduled on the Monday for a 20 week ultrasound for anatomy scan and to confirm it was a boy. Instead on that Monday I had a D & E because after being in labor all weekend, the baby did not deliver. My doctor was out of town too. It was a long time ago, but it was painful for me (mostly emotional) definitely some physical too. We have three healthy daughters now, but I totally understand what people go through and it’s a sad experience. Thanks for writing the blog, I feel like doctors don’t really educate very much on this subject. I had my losses 16-22 years ago, though, maybe the physician education is different now.
Thank you so much for sharing your story with us! I know there is a push in education for doctors on dealing with patient grief, but I also know that they’re so swamped with patients that it’s hard for many of them to put those lessons to use. I think that’s a lot of the reason that we’re seeing more and more patient advocates in the medical field. It’s an attempt to make sure patients feel like someone hears them and has empathy because doctors are just so overwhelmed. My experience with recurrent pregnancy loss opened my eyes to so many problems with medical institutions in the US, most of which are not actually the doctors’ faults. Again, thank you so much for sharing!
I experienced a loss end of November I was exactly 13weeks I was due for my sonogram that did all the measurements and such the next day
And ur totally right
I didn’t have anything for my daughter and it was exactly the same just a little less intense Physical pain but the emotional pain was much greater so I feel it over all evened out
I feel like this is a subject that’s very taboo and people don’t talk enough about it to understand what is involved with it and often brush it off like it’s nothing So I feel like it’s very important to I have people understand a bit better
Thank you so much for sharing! What a unique perspective you bring from the unmediated end of both spectrums!
I experienced a miscarriage with misoprostal after finding out at my 9 week appointment that I had a blighted ovum, and I would choose D&C if it happened again. I had very heavy bleeding the night I took the medication (as expected) and then it turned into a heavy manageable period. Unfortunately I woke up in the morning three days later to another bout of unexpected heavy bleeding and cramping. I was stuck in the bathroom for over an hour with bleeding so heavy I couldn’t leave the toilet. Then, I had another bout of heavy bleeding (though not quite so bad) 6 weeks later. After I had already had a regular period. I didn’t think I was pregnant before that but was convinced I was having another miscarriage (blood results from the next day confirmed no HCG, so it was residual bleeding from the original miscarriage). I wish I was made aware of the extended timeframe a misoprostol miscarriage could have. Also the pharmacist definitely judged me. I said the doctor had called it in but I didn’t know what it was called, but I would recognize the name. She said she couldn’t even begin to try to pronounce it (it’s not that hard). When I asked her to just try she said “it’s the abortion pill”.
Oh how I want to punch that pharmacist in the effing face! I am so sorry for your experience but so appreciate your story. I had heard these stories, which is why I chose a D&C, but I know there are bad stories about those as well. Thank you so much for sharing. I know your story will help other women!
What this article does not go into is a fourth (in my opinion) type of loss. The loss when a frozen embryo transfer (FET) from infertility treatments is done. I have now had 4 pregnancies lost and the loss from my FET was my worst.
My first pregnancy loss I took the medicine to induce the loss. It was the most painful experience due to the severe cramping. I took the pill and within 12 hours I was laying in a bathtub having the worst pain of any loss. I was lucky in that it worked well for me without any complication and the pain subsided after the first 12 hours.
My second and third were natural losses, that I fell lucky were not extremely painful, other than the emotional aspect.
After the third loss my doctor referred us to a specialist where we did fertility treatments.
A little about a FET cycle. You start a pill 3 times a day on cycle day 2-4. You go get an ultrasound and they check the uterus and the ovaries. Making sure everything is calm and relaxed. You continue taking these pills for weeks. You extend your cycle, you build what is called a triple thick uterine lining. 7 days before the transfer you start shots into the backside, 6 days you start what I will call an insert twice a day. Both of these meds are progesterone. I am now tricking my body into thinking its pregnant. My embryo is 6 days old so my body should be producing this but can’t because my embryo did not grow in me. You continue to take all these meds and you wait. 10 days you wait. Then you take a blood pregnancy test and you know that day if it worked or not. They whole process takes weeks and weeks.
For me the blood test came back positive but with low numbers. We were to retest in two days and as long as they were doubling we could consider the pregnancy viable. You keep taking the meds. Two days later I had a negative blood test. Time to stop all meds. Time to let nature take its course. Here is the rough very rough part of an FET loss, you build this crazy thick lining before they even transfer, so you’ve tricked your body into being further along then the actual time the embryos was there. And you have to shed that and come down from the hormones. The shear amount of blood loss was terrifying to me, not to mention the cramping and emotional aspect. I share this because not many share their IVF and FET stories because its not easy. The way this weighs on my heart four months after the loss make me choke and tear up typing this. But I wish I would have know what that FET loss was going to be like. I thought I had been seen it all after 3 losses but I wasn’t even close.
Oh, Cynthia, I am so sorry for your experience, bud I SO appreciate your comment. Because I’ve never experienced IVF, it’s not something I can speak to, but I know it’s something so many women need to hear about and can relate to. I’m so thankful for this comment. If you’d ever like to write more about your IVF experience, I’ll welcome a guest post from you. Sending you so much love!
I had my first miscarriage at 6 weeks, chalked up to a nasty dog bite I got. It wasn’t anything more than a heavy period for me. My second miscarriage was at 10 weeks and I have never felt pain like it. Even Endone couldn’t numb in pain of the contractions. Two pregnancies lost and a lot of hope lost with it
I’m so so sorry for your losses! It’s such a hard time to go through, and the waiting for testing, if you go that route, feels so long. But statistics are on your side if you choose to continue trying. So much love to you ????????????????
I had a missed miscarriage. On Friday we went to the doctor for our first scan only to be told the gestational sac was empty. I was sent to emergency gynaecologist service and was given 2 choices. D&c or misoprostol. Tbh I was in no shape to make any decision at that point. My partner made the decision based on the doctors recommendation for misoprostol. They did a blood test to make sure there was no anemia. About 2 hours waiting for the results the hospital called us back in and a nurse inserted 4 pills into my vagina and they sent me home with a follow up appointment for next week. About an hour after leaving the hospital the pain started and I miscarried that evening. The pain is horrible much worse that period cramps. I can’t walk for long and I’m on prescription pain killers. The blood was only heavy for the first 24 hours and now is more like a heavy period. But the pain is the worst.
I’m so sorry you’re going through this right now, and that the Misoprostol worked well for you. Not that any such story is “good,” but I love hearing successful stories about it because I hear so many bad ones. I don’t think that’s because it’s bad, but because people talk about negative experiences more. Thank you for sharing, and please reach out if you need an ear! Love to you!
Thank you, Katy! This is so honest but also so kind. I needed this when I miscarried my first pregnancy and felt so afraid and alone. I miscarried again after the birth of my first daughter and that time I knew I needed to talk about what I was experiencing and going through. This is essential information and critical work. Keep it up, Lady!
Thank you, dear! I searched far and wide for this kind of information during my recurrent pregnancy loss journey! I only hope others can find it when they need it ????
I’ve had 2 losses. My first was at 20 weeks 2 days. Call it intuition, but I knew something was off with that pregnancy from the beginning (it was my third pregnancy). We had a healthy ultrasound at 10 weeks, but at 16 weeks my doctor had a very hard time finding a heartbeat. He did find it, but something was off. We went in for our next appointment and couldn’t find a heartbeat. We already had our ultrasound scheduled for that afternoon, and it was confirmed our baby had passed. I was sent to the hospital where they inserted misopristol. I started having some cramps. I was given 2 pills every 4 hours to take orally. After the first oral dose my water broke, and after the second oral dose my son was delivered. I was then given another 2 doses and a shot of oxytocin to deliver the placenta. I definitely was in labour with him, but it was nothing like my previous 2 labours (all 3 were without any pain medication).
My second loss was a blighted ovum at 7 weeks. At 5 weeks I had some spotting that lasted a week. At 6 weeks I passed a couple clots, then the bleeding stopped but I had zero pregnancy symptoms. Again, call it intuition, but I knew I was going to lose that pregnancy too. I went to my doctor who ordered HCG levels and an ultrasound. My HCG didn’t change, but the ultrasound showed the gestational sac, measuring 4w5d. My doctor wouldn’t do anything to start a miscarriage until my HCG dropped, but I started bleeding that weekend. On Saturday it really was just a heavy period, but Sunday was worse- I was nauseous, my whole body ached, and I had pretty intense cramps. I passed the sac and everything eased up almost immediately. I bled for another 4 days once the sac was passed.
Thank you so much for sharing your experiences. I’m fascinated that your doctor wouldn’t do anything until your HCG dropped. With my BO, my doctor wanted to intervene specifically bc it was doubling normally and my sac was growing normally. Different experiences are so fascinating!
When I was about 8 it 9 my mom found out she was pregnant, which she was excited about but also terrified because at the time she was also at the tail end of her beating breast cancer and having both breasts removed. Her doctors told her that she could be at great risk because of the chemo and such but she decided to see if her body could bring her another child to love.
Sadly a few months later they found out it was a tubal pregnancy and that it had become infected and her whole uterus had to be removed. I remember her telling my brother and I that even though we never got to meet this new baby that she was glad we had a little happiness after the horrible 2 years of her fighting and beating cancer and I’ll never forget that.
Oh, that’s so much to go through at once. It sounds like she had an amazing attitude about it, but how much for her body and heart to deal with. And yours!
Thank you so much for writing this thorough post on what to expect from your body when you are miscarrying.
When I discovered I had a missed miscarriage at 10 weeks (read my full story here: https://mamarissa.com/my-beginning-of-motherhood-miscarriage/), I was soaking up every bit of information I could find on what to expect physically and emotionally.
I am so sorry to all my fellow mamas who have experienced a miscarriage. It is so heartbreaking.
Thank you for this helpful comment and article! Shoot me an email at katy@undefiningmotherhood.com. I love what your site is doing and would enjoy chatting about ways to collaborate!
My partner and I have been struggling to get pregnant for a few years now and have had to proceed with IVF. At first we tried IUI and then after that didn’t work we started the IVF process. We did one fresh transfer, which did not take, and then we tried with a FET. That was successful and we saw what we were told was a strong heartbeat right around 7 weeks and that we had a viable pregnancy. Then around 10 weeks we had another ultrasound and were told there was no heartbeat and that the baby had stopped growing 2 days after we saw the heartbeat. I had never heard of a missed miscarriage before and everyone told me prior to us finding out about the miscarriage that if there was no cramping or bleeding we shouldn’t worry. It was devastating after trying for so long to not only have the miscarriage, but to continue thinking for 3 weeks that everything was going fine because my body didn’t display any sort of symptoms that I had read about. We are now pregnant again currently at 11 weeks, but every day is an endless worry about potentially having another missed miscarriage.
Thank you so much for sharing your story, and I’m so sorry for your loss. Pregnancy after loss is SO hard. We have some articles about coping that may be helpful. 🤞🤞🤞 for your!!!
On June 21, 2020 Father’s Day I found out I was pregnant. I was shocked and had taken another 7 more test to make sure. I was extremely happy and excited to be pregnant at 40 years old and 10 years later of having my daughter. I told my boyfriend who was excited as well. We started making plans and had both boy/girl names for our baby. On July 3rd I was rushed to the hospital cause I had spotting of light red blood. I was crying and nervous, worried but praying my baby was okay. Once in the room, the nurses took my blood, urine and did both ultrasound and vaginal done and a swab to make sure the baby was okay. I was told the gestational sac is there but no baby, it’s too early to see so they discharged me. My appointment with my OBGYN doctor was two weeks later. When I saw him, no blood work was done and was told you can schedule to have another ultrasound done to make sure there is a heartbeat. I made the appointment for the next day. I was excited and couldn’t wait to get pictures of my baby. At this appointment I was questioned prior to having the ultrasound done and was told I would get a call from my doctor. I answered all the questions and was confused to why am I being questioned and why will the doctor call me after the ultrasound. While having the ultrasound, the tech didn’t explain anything to me or gave me any pictures and just told me, your doctor will call you. Once again I was confused, why am I being told this. Two minutes after leaving the imaging office a nurse from my doctors office called and told me my baby had stopped growing at 5 weeks and there was not heartbeat. I couldn’t comprehend what was being told to me, I asked what’s wrong with my baby and then the nurse said you had a miscarriage. My heart broke, I was very emotional and couldn’t believe what I just heard. Then I was told you will pass it over the weekend and I’d not just come to your appointment on Monday with questions. I was hurt, broken, upset by the way I was treated. I called my boyfriend who was also upset and nothing made sense to him and we decided to go back to the hospital that night to get better information and to make sure they were right. At the hospital they did another ultrasound and once we were told, there is no baby in the sac and it was a chromosome that didn’t match. We left thinking our questions were answered but I felt in my heart something wasn’t right. I decided not to go through with the D&C and went to a different hospital, once again had two ultrasounds done and was told that there is a baby in the sac. My boyfriend and I was shocked and happy. I was recommended to see the OB doctor that works there and I did. When I saw her, she couldn’t give me definite answer since she didn’t have any records to go by. She scheduled me to have an ultrasound done in her office the following week. The ultrasound there did show that my baby was in the sac on the upper part of the sac hiding but unfortunately no heartbeat. I had a Missed Miscarriage. It hurt so much to see and hear that but I was happy I waited to know my baby has been there the whole time. It took four doctors for the last two to actually see that my baby was there. I did end up having the D&C last Thursday. Didn’t know what to expect and it has been painful, sleepless nights and very emotional. It has been a roller coaster for my boyfriend and I. I pray that I heal soon from this and we will try again.
I’m so sorry for all you’ve been through. The emotional healing process is so hard, not to mention when you’ve gone through months of confusion and the physical struggles. So much love to you!
I wish I had found this a couple weeks ago when I started miscarrying. At 8 weeks pregnant I was given almost no information about what I should expect during the process. A “heavy period” warning did not at all prepare me for anything even remotely resembling a baby to show up in my underwear.
I’m so sorry for your loss and experience. It can be so incredibly traumatic. How are you holding up now? Sending you so much love!
I’m crying reading every comment and the whole article. I cannot thank you enough. I’m a week out from taking “the abortion pill” to clear my missed miscarriage at 10 weeks. I’m one of the ones who went through all that came out. I saw her and I’m so sad every day. Still bleeding , still cramping and back pain. I was rushed to the ER from blood loss and very close to having to get a blood transfusion from the blood loss of the 4 pills I steered into my vagina. I never ever EVER recommend this to anyone. This is my 2nd. Been trying 17 years and I’m almost 40. First was jan this year at 6 weeks. Much like a heavy period. This last one was hell , mentally and physically. I give up. I don’t feel alone after reading this article and I’m so so thankful. 2020 sucks all around. God bless everyone.
Oh, Lizzie! Sending you so much love. This is SO hard, but you are absolutely not alone. Reach out anytime you need to talk. The easiest way to reach me is on Instagram @undefiningmotherhood
Thank you for this article!! I just went through a missed miscarriage last week and needed this. Due to cost and timing due to Covid, a mutual decision was to take cytotek (I was 8 and a half weeks). Doctor said statistics for cytotek are 71% successful on first dose and 85% successful on second dose. My husband and I felt confident with that route and rearranged our schedules. First dose left me with one long unbearable cramp for 1.5 hours and then contraction like cramps for another hour after with minimal to no bleeding. After 13 hours from first dose, I needed to take the second dose for miscarriage to be successful. Again major cramping (this time I had oxycodone) in a more contraction like manor but just as bad as first dose. This time I had more bleeding but very similar to a typical period. I never understood how much tissue would be passed so I assumed all was done when cramping stopped. Bleeding kept up with bits of tissue but I was able to work again. A couple of days pass and cramps begin ramping up again over the next 36 hours ending with unbearable cramps and double oxycodone (dr approved). Heavy bleeding and MAJOR tissue passing. I’ve never had pain like this before and would never wish this on anyone ever!! Finally I think it’s all over but there is an uncertainty to all of it. The dread of more cramps to come. Looking back, I definitely should have gone to the hospital for an emergency D&C but at the time we didn’t know if all of it was good/bad or right/wrong. I spent more time on the toilet than with a pad so I didn’t know how bad the bleeding truly was. If anyone ever has the choice, my strong first recommendation is to NOT take the medication. It was not only hard on me but my husband as well. We have both decided that (hopefully not) but IF we have another miscarriage, we will go the D&C route.
I was 16years old when I found out I was pregnant my family didn’t believe I was intel my now ex boyfriend told them theirs Hight changes! My family wasn’t not the happiest person in the world. But than they didn’t know I was hurting as wall. I was scared I didn’t know what to how to rise a kid I am only 16 don’t know what too do! And it also didn’t help 3days after my boyfriend out I was pregnant he broke up with me! and started a rumor that I wasn’t and if I was he would make me get arbutin.
2week I found out I was pregnant my best was also 15weeks and she found that she miscarried and SHE couldn’t have anymore kids at all because of it. I was scared I was hoping that I don’t
3weeks later so at this point I was 5weeks almost 6weeks along so out of no where I was bleeding really bad and idk y so I looked it up on google and I asked my best friend she told me that was normal if its gushing and cramp really bad go to the E.R that ant good She also told me that the bleeding only last few hours to 3days! and the blood has to spotting and brown or pink…
5days I was still bleed but this it was bright rad and it was coming fast and I also had sharps pains they felt wore than a cramp!
I was in the middle class when I felt big rush of blood coming down and I want to use the bathroom to see what was going with my body and I got on the tole and doom SOOO much blood and than I looked down I seen this thing that looked like what the baby is at 6week on pregnancy’s tracker! I started to cry my eyes out. I Now I lost the baby it worst day of my life. I walked back to class in pain and I didn’t need to go home I only had 10mint left and my guy friend asked me why I was crying and than I didn’t now what to say or anything…
so want home and looked miscarry and I had everything I did not say anything family. I never thought losing a baby as teenager can hurt but it can so much and now know the father of the my baby I told him and cried and he apologized for telling to get darshan and that baby don’t need to now us it don’t have feeling. But that’s wrong It has life to live… than ones I lost the baby he lost him self to.
Right now I wish that I get to see what my gander would be what the baby would be watch it grow up. I am very sacred to have kid and than end up losing it again. even miscarry as teen it still hurt but little worse it kind of makes us not want to have kids anymore. I kind of now I have 2friends that got pregnant 2 and miscarry them both and their sacred to have kids like me…..
IFY :Teen don’t have sex broth Control doesn’t work as wall as combos I Used both and I got pregnant