Misoprostol is often called the “miscarriage pill,” as it helps women who’ve lost a pregnancy actually expel that pregnancy from their bodies. So yes, it’s as gross and horrifying as it sounds.
It’s the generic form of a drug called Cytotec, used to induce miscarriage. In this article, Arden Cartrette discusses her terrifying misoprostol experience, the timeline of her misoprostol miscarriage, and why she wishes she’d read other misoprostol stories before taking it for an incomplete miscarriage.

This site contains affiliate links, meaning that we earn a small commission for purchases made through our site. We only recommend products we personally use, love, or have thoroughly vetted.
Arden’s Cytotec Story
When the doctor said the words “I’m sorry but it looks like there’s no heartbeat,” it confirmed our worst nightmare. A second miscarriage. I was in a state of shock.
With our first miscarriage, I opted for a dilation & curettage (D&C) right away because the thought of going through a miscarriage at home was terrifying. Ultimately, my body had a plan all along, and I miscarried naturally, at-home, the night before the scheduled procedure.
As the doctor was confirming our second loss, I kept thinking about how I really wanted it to be over as soon as it possibly could be. So I asked him to prescribe me the miscarriage pill and told him that I would induce the physical miscarriage at home.
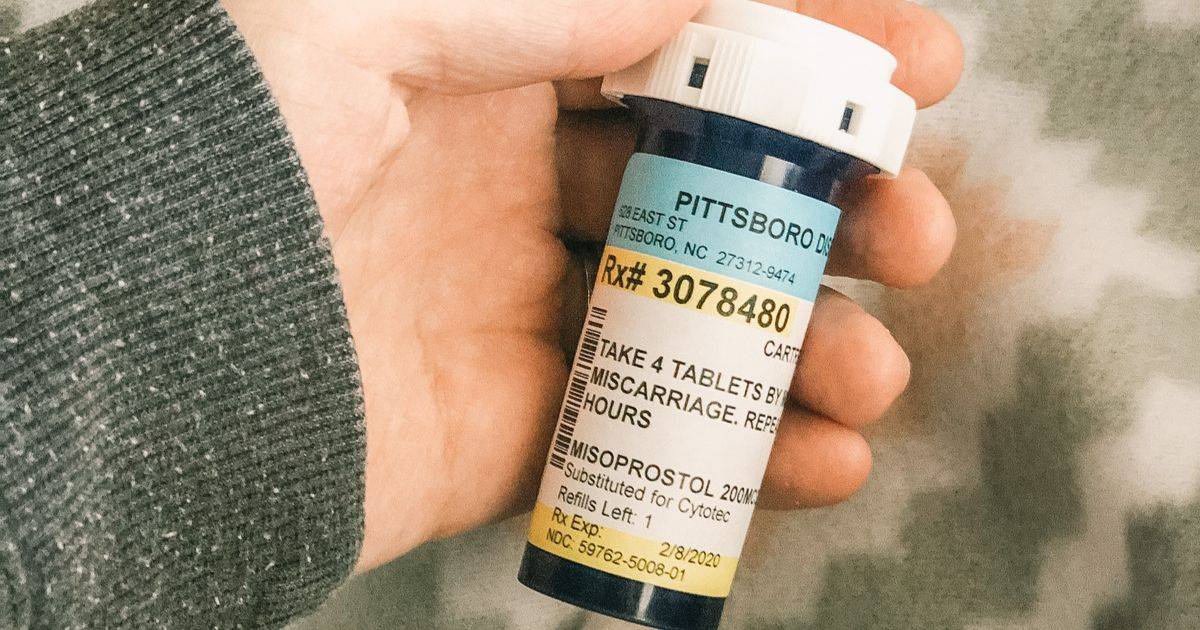
The “miscarriage pill” medication is called Misoprostol, which is the generic version of Cytotec.
What Is Misoprostol?
Misoprostol is used to help the body complete a miscarriage.
“Misoprostol has been used off-label for many years as a safe and effective treatment for first-trimester incomplete miscarriage. Misoprostol binds to smooth muscle myometrium and causes uterine contractions.”
American Academy of Family Physicians (AAFP)
This causes the body to let go of the pregnancy, which is helpful in the case of a missed miscarriage, when the body doesn’t recognize the loss and miscarry naturally.
(Editorial warning: If you see your medical chart, this might be labeled a “medical abortion.” This is standard medical terminology and has nothing to do with how wanted your loss was. Learn more about the medical term for miscarriage here.)
The AAFP definition of Misoprostol is “safe.” Still, if you read the drug information, you’ll see that misoprostol side effects can be VERY extreme.
Effects of misoprostol may include heavy bleeding and clotthing, to the point that you require medical attention. Call your doctor for advice about the amount of bleeding. It’s a great way to help with reducing the risks associated with misoprostol.
Plenty of people have good experiences using Cytotec for miscarriage, but there are also plenty of horror stories. Being educated about the drug will help you manage.
Personally, my misoprostol experience was horrific.
Is Misoprostol Safe for Miscarriage?
When you are told that your baby is no longer growing and that you should prepare for a miscarriage, you are normally given three options.
While no option is better than another, being educated about these decisions allows us to make the right decision for us.
To carry out a miscarriage, your options are:
- Waiting for your body to catch up and letting it happen “naturally”
- Taking a Misoprostol to induce the miscarriage
- Scheduling a D&C where you are put under general anesthesia while the tissue is removed from your body
At the time of my second miscarriage, I thought that I was making the right decision because taking Misoprostol would give me control, and I desperately needed some control.
(Editorial note: This thought process shows how different the experience of miscarriage is for everyone. When given the choice, Katy elected to have a D&C because she thought using misoprostol for incomplete miscarriage felt too uncontrolled.)
My journey felt out of control because things weren’t going as I planned they would.
But that’s just what a fertility journey is: unplanned chaos.
However, I wish I had known then what I know now about taking Misoprostol–side effects, stories, bad experiences, and all.
While it is deemed “safe” for inducing miscarriage by organizations like the American Academy of Family Physicians, that was not my Misoprostol experience.
My Misoprostol Experience
After I asked the doctor for misoprostol, often known as the miscarriage pill, he sent me on my way, and I planned to take the four tablets to induce the miscarriage the next day.
Saturday, February 9, 2019, at three o’clock in the afternoon.
I chose a specific time so I would hold myself to it.
It gave me the morning to say goodbye, do whatever I needed to do, and then I could have some control over when the worst would happen.
I set an alarm on my phone, went to the nearest store, and bought essential items like maxi pads, and adult diapers.
Although I felt hurt and confused,I just wanted this to be over.
I was tired of constantly feeling like I was pregnant and miscarrying.
For the past six months, that was all my life was, and after a year-and-a-half of infertility, I was fed up with things not working out the way that I thought that they would.
How Was I Supposed to Take this Miscarriage Pill?
When three o’clock came around, I held the four tablets in my hand and prepared to take them.
They symbolized the physical end of my second pregnancy and still, I had nothing to show for it.
How was I supposed to willingly take a medication that would evacuate a pregnancy from my body?
How was this happening to us, again?
It didn’t seem real.
My husband, Kerry, sat next to me on our couch as I prepared to take the medication. He reminded me that this wasn’t my fault and that soon the physical part of this loss would be over. He reminded me that I wasn’t in this alone and that was reassuring, but as I took the tablets one by one, I couldn’t hold back my tears.

Once again, I was afraid for my future.
Could I handle another miscarriage?
Would I ever have a healthy pregnancy?
The first step to finding out the answer to either of those questions was to take the medication, so that’s what I did.
My Misoprostol Miscarriage Timeline
Roughly an hour after taking the misoprostol, the cramping started.
As a woman with semi-regular periods, I knew that first came cramping and then came bleeding. Another hour later, I noticed that the spotting had begun.
I excused myself to the bathroom so that I could labor and miscarry.
The miscarriage took six hours and, after what I thought was the worst of it, I lay in bed with a heating pad and cried.
I thought it was time to recover and heal.
Three Days Later, the Pain Intensified
I returned to work three days after I took the medication. By that time, I was ready for a distraction from my miscarriage experience.
Sitting at home was lonely and filled with reminders that I was no longer pregnant. I didn’t want to be there anymore.
The day that I went back to work was a Wednesday, which is also the one day of the week that was the busiest in our office so there was more work and running around for me to do than usual.
Around mid-afternoon, I noticed that my cramping was intensifying and the bleeding was getting heavier.
Assuming I had just overworked my body, I excused myself to go home early to take a hot shower and lie in bed with a heating pad.
After Kerry and I ate dinner, the pain had become so intense that I felt like something had to be wrong.
My first miscarriage happened in a few hours. In the days that followed, I was sore, but my bleeding hadn’t picked back up like it was this time.
Once I noticed that I was having to change my maxi-pad every 30-45 minutes and that I was now passing blood clots, I told my husband that we should go to the emergency room.
Something just didn’t feel right.
(Editorial note: When having a miscarriage, the general rule of thumb is to go to the ER if you are soaking through a heavy maxi pad per hour, or more.)
Misoprostol Side Effects Landed Me In The Emergency Room
I will never forget the moment that everything seemed to take a turn.
If I’m being honest, this moment alone left me with post-traumatic stress disorder (PTSD) that I struggle with to this day.
The physical feeling of passing tissue and bleeding through layers of clothes is something I wish I could erase from my memory, but it’s stuck with me.
Once we arrived at the ER, I got out of the car to go through the double doors where I would check-in and start the triage process.
I felt the most intense pressure, and I could tell that I had just passed something that was very large in size.
Next, I felt something wet run down my legs.
I was wearing an adult diaper, a maxi pad, men’s briefs (trust me, after a loss, they are so comfortable), AND sweatpants. I could feel the wetness through ALL of these layers.
It had soaked through all of those layers and blood was now running down my leg.
After we checked-in, I ran to the bathroom and started to sob.
I had passed tissue that was larger than anything I had seen in my experience with miscarriage and there was blood all over me. What was happening?
I Was Overwhelmed by My Experience with Cytotec for Miscarriage
It didn’t even occur to me that this could be part of the miscarriage because I thought that the physical aspect of our loss happened three days prior.
Over the next sevenish hours, I sat in a hospital bed in the ER and bled. A lot.
The nurses and doctors were all very nice, but it seemed that no one understood what miscarriage was like.
They kept asking me how far along I was, and I explained to them that I was 7 weeks but had recently been diagnosed with a blighted ovum.
I could tell that when they heard “7 weeks pregnant,” they assumed that the bleeding couldn’t have been very much, but they were wrong.
I kept explaining that the blood clots were the size of lemons or larger, that the blood was soaking the very small and thin pads that they kept giving me. I even had to argue with a nurse to get something other than Tylenol to help with the pain.
(Editorial note: knowing how to advocate for yourself as a patient is essential during miscarriage. Learn more about patient empowerment.)
I was in a hospital filled with people who save lives, but I felt like I was the only one caring for my situation.
After we had been sitting at the hospital for five or six hours, the OB resident came to see me and said that, because of my blood loss, he recommended I have a D&C.
I agreed and just wanted this to finally be over. I was tired, sore, in pain, and I felt dirty from all the blood that was on my legs, lady parts, shoes, etc. Please, do whatever you need to do to end this, I thought.
We Finally Returned Home, but the Questions were Just Beginning
Kerry drove me home a few hours later. I hoped that this was FINALLY the time that I could rest.
Emotionally, mentally, and physically, this miscarriage took everything out of me, and even though it seemingly was over now, I felt confused about what had just occurred.
Why did my miscarriage start and stop over the course of a few days?
Did I do something wrong by taking misoprostol for miscarriage?
Was this experience normal?
My doctor didn’t require an immediate follow-up and had a full schedule until about a month after the loss, so it would be weeks before I had some answers.
Mine Was Not an Uncommon Misoprostol Experience
A month after the traumatic night in the ER, I had an appointment with my doctor, who was our fertility specialist.
Because we had struggled with infertility prior to our first pregnancy and now suffered two miscarriages, he was our main point of contact.
When I told him about my hospital visit and experience, he wasn’t surprised.
Apparently something like 60% of women who take misoprostol has to have a D&C and/or have complications like hemorrhaging days after what they think was the miscarriage.
(Editorial note: Undefining Motherhood has not been able to find the research to support this claim, but Katy’s OR nurse told her the same thing when she went in for her D&C.)
Why did no one explain this to me? I thought.
I would have never taken the medication had I known that this was a huge risk.
In my head, taking the misoprostol gave me control, and that’s why I had chosen to take that route. But in reality, it threw me into an extremely uncontrollable situation.
We Need To Talk About the Ugly Parts of Misoprostol for Miscarriage
I quickly learned that no one tells you the ugly parts of miscarriage because they think you are fragile. (And they aren’t wrong).
However, your doctor has an ethical responsibility to warn you if something like this can happen.
No one told me what to expect when you miscarry before my first miscarriage, and I assumed that because I made it through that, I could get through anything.
Looking back, I wish I had asked more questions and had taken more time to think over my options instead of acting quickly. I wish I had read more misoprostol stories.
I was simply trying to choose the option that I thought would make this miscarriage end the quickest.
My doctor should have advised me about the potential misoprostol side effects in order for me to have made a more fully informed decision.
And that decision would have been NOT taking misoprostol for miscarriage.
What I Wish I Had Asked My Doctor About Misoprostol
If you’re ever in this situation, I hope you’ll find these questions helpful as you navigate this decision. Don’t be afraid to ask your healthcare providers questions.
Don’t be afraid to advocate for yourself.
- What is the success rate of only having to take one dosage of Misoprostol?
- Out of every 5 miscarriages that you diagnose, how many women choose the medicated route? And how many of those women have success?
- How does inducing the miscarriage with Misoprostol differ from letting it happen naturally? Which is a safer option? (The answer probably depends on your gestational age, as well as how long it takes for you to miscarry without intervention.)
- Can I start with a lower dose of Misoprostol in case my body has a reaction to the typical dose?
- What are concerning misoprostol side effects that I should look out for? At what point should I begin to worry about said side effects?
My Advice For Choosing The Best Option For Your Miscarriage
Since I’ve now gone through two miscarriages (although one of the miscarriages was more like two in one), I’m familiar with all of the options because I’ve experienced them all.
I often wish I could go back in time and give myself some advice instead of acting quickly and trying to take the route that I thought was the quickest.
Here are some tips for choosing your options on proceeding with the physical miscarriage:
1. Sleep on it
Yes, I know that this is a typical thing that people tell you to do when you are faced with a difficult decision, but it’s underrated. I took only a few minutes to decide what to do, and I wish I have talked more about my options with the doctor that day and taken at least 24 hours to think it over.
When you are told that you’ve miscarried and have to plan to do so physically, your mind can’t focus on the information in front of you.
All you hear is, “Your baby isn’t alive” and you can’t think about anything else.
Take the rest of the day, sleep on it, and call your doctor’s office the next day with your decision. Don’t act on fear or impulse.
2. Ask questions
Don’t be afraid to ask questions or to call your office back with questions the next day.
This is your body, your child, your fertility, and you have every right to ask any question that pops into your head.
3. Find support (including through online communities)
Something I did with my first miscarriage, but not with my second, was asking about others’ experiences with miscarriage.
I was a part of a Facebook fertility support group at the time, and I found a lot of comfort in hearing others’ stories about their losses.
People still held back on the details, but it was oddly comforting (and terribly heartbreaking) to hear their stories and see that I wasn’t alone.
Also, think about what it might’ve saved me had I heard more people’s scary misoprostol experiences. Because it turns out there are a lot.
4. Talk with your partner
Although, as women, it’s our body that goes through the physical miscarriage, our partners should have a say and can actually offer helpful advice, too.
After you learn about your options from your doctor and decide to take the day to think it over, talk with your partner and make sure that you are both on the same page.
5. Think through the finances
It goes without saying, but make sure that you can afford whatever option you choose.
In our case, we have a high deductible insurance plan so paying for a D&C would have cost us thousands out of pocket.
That said, it turns out an emergency room visit cost double what the D&C alone would have cost.
Know your medical benefits and coverage and make a decision that works for your family and finances.
Miscarriage is hard enough. Don’t let it take away your financial freedom, too.
Misoprostol Stories Can Be Different
Any time I share my Misoprostol story, I like to remind others of one thing: just because my misoprostol experience was negative doesn’t mean that all experiences will be like mine.
I’ve met women through the online miscarriage community who had a “normal” experiences taking Misoprostol for miscarriage. Many women have no issues and are happy not to have paid for a D&C.
Alternatively, some women have reached out to me and shared that they had to take 2-3 doses and ended up having a D&C.
The truth is, anything with healthcare (and fertility) depends on the person and their situation.
But I share my misoprostol experience with you so you know the possibilities. Because had I known the high percentage of women who had negative experiences, I don’t believe I would have opted to take the Misoprostol.
If you’ve experienced what I have and felt let down by your body, your doctors, the healthcare system – just know that you aren’t alone. I see you, hear you and feel for you in every way.
What was your Misoprostol experience like? Tell us about it in the comments.

General FAQ
Is misoprostol safe for miscarriage?
Generally, yes. It’s considered safe to induce miscarriage and is often used to induce the miscarriage in the privacy of a patient’s home without a healthcare professional. Personally, I think that it should only be used in a medical setting such as a hospital or doctor’s office. I wouldn’t recommend a friend choose this option, especially at home alone.
What to expect after taking misoprostol?
Many doctors will tell you to expect a heavy period after you take the misoprostol. But like any miscarriage, a “heavy period” is usually a major understatement. Physically, you can expect cramping, bleeding, blood clots, intense pressure in your vagina, pain, and potentially vomiting from the pain.
How long does misoprostol stay in the body?
The half-life of misoprostol is only 20-40 minutes. But, as with any medication, traces can remain in your system for a long time.
How long does it take for misoprostol to dissolve?
There are a few different forms of Misoprostol. One dissolves under your tongue or can be placed near your cervix and left to dissolve or you can take the medication by mouth. Placing the tablet near your cervix helps the medication act faster, but many doctors recommend taking it by mouth.
Other Miscarriage Stories
- Beth’s ectopic pregnancy story
- Katy’s recurrent miscarriage success story
- Back-to-back miscarriages: Whitney’s story
- A story of fathers dealing with miscarriage
- Dawn’s unplanned pregnancy miscarriage story
- Katy’s blighted ovum story: what to expect + symptoms
- Natasha’s experience miscarrying twins
Miscarriage Articles
- Miscarriage tattoo ideas
- What to expect when you miscarry
- Recurrent miscarriage testing
- Coping with miscarriage grief
- Creating a miscarriage memorial
- What to do after miscarriage





Hello! I’m so thankful to find your blog post. I recently had almost the exact same experience going to the ER 7 days after what I thought was the end of the process after taking the pills. No dice. I’m right there with you with the ptsd. With Covid-19 going on D&C was not an option. They didn’t give me an option at the ER either. They basically said this was normal and good luck. Really happy to spend all that money for nothing. Anyway thank you for sharing, it helps to know we’re not alone. I hope you’re doing well and staying safe!!
I had a positive pregnancy test on July 9th. Me and my husband had gone through fertility treatments for 2 years (5 failed IUI’s and shots every other day for him). We conceived w/o IUI, he had been on gonal f for 6 weeks. I was shocked, as I thought we would live life without children. I was so happy and experienced all the pregnancy symptoms (sore breasts, nausea, bloating). I went in for my 1st ultrasound on August 3rd, which would put me at 8 weeks. Due to covid, my husband couldn’t be there with me. I was crying tears of absolute joy when I saw the baby on the screen, but those tears quickly turned to anguished sobs when the nurse said quietly, “I’m sorry, there is no heartbeat.” Baby was measuring at 7 weeks. I had another US the following week to confirm. No growth, no heartbeat. My nurse went over the 3 options. Natural, medication or D & C surgery. I waited 3 weeks to go the natural route. My doctor finally said I needed intervention. I decided to go with misoprostol. The D & C sounded too invasive and risky to me. I scoured the internet for women’s experiences with it. I also spoke to complete strangers about their experiences. I found it so helpful and I think it’s what got me through. I took 4 miso vaginally at 5:30pm Sunday night. I had taken ibuprofen, oxycodone and zofran 30 minutes before insertion. I began bleeding at 10pm and between 10:30pm-2:30am I had non stop contractions. Worse pain of my life and the pain meds did nothing. I had a heating pad and just moaned and groaned and begged God to take my pain away. 4 hours later the cramping subsided and I was able to sleep. I had passed some tissue, and dripping blood in the toilet, but was not soaking through a pad an hour and did not feel dizzy or faint. The following day I felt something slipping out of me, and it was just dangling there. I called my doctors office and they said I could pull it out gently, which I did, which did not cause any pain. I knew it was my baby. I wrapped in up and put it in a box and will bury it. I have an ultrasound on Friday to ensure everything is clear. I hope I am because I don’t want a D & C. Even though it was the most awful pain I had gone through, I would do it all again. I felt strong after and I think talking to others and learning their experiences helped me get through this myself. Please research and talk with others and decide what’s best for you. Every woman is different and experience is different.
I am so sorry you had to go through all of that!! Unfortunately, my story is very similar and happened last week! I was 8 and a half weeks along. Baby passed away only 2 days before going to the doctor for our first visit so my body had no idea anything was wrong. Hearing those words really do shake you to your core. My doctor did not advocate for one remedy over the other so my husband and I opted for the cytotek due to cost but also I didn’t want the potential chance of scar tissue to be an issue for future pregnancies. Doctor said the success rate for first dose is 71% and 85% for second dose. There was a chance we would have to have a D&C but it was a chance we were willing to take. I took the cytotek vaginally the next day and my thoughts were the exact same. How can I take this medicine if I want this baby so badly? I didn’t want them to go away but I had no choice and that alone was the most awful feeling. After immense pain and contractions for 2 days straight and not tons of blood or tissue, I honestly thought it was over. 3 days later cramping began to ramp up and the 4th day was the worst. Cramps were so bad that 10 mg of oxycodone didn’t even make a dent in the pain. 2 heating pads, 2 blankets, my husband rubbing my back and a throw up bin while sitting on the toilet was my life for an easy 2+ hours. A large amount of tissue was finally passed at once and the pain immediately began to subside while the dizziness increased. It was all I could do to keep my eyes open after that and just passed out on the couch. That seems like the end but I cannot be certain that pain won’t begin again in a couple days. Cytotek is no joke and I definitely will never choose that option again if we have another miscarriage. As far as anyone I know or anyone that hears my story, I will never advocate that medication due to the complications I had. It is 100% their choice and I hope whoever they are, they know they have my support regardless of their decision because the best thing in the moment is having support. That entire week has been the hardest and scariest week of my husband and I’s lives and I pray for anyone who ever has to go through a similar experience regardless of the remedy they choose! Here is to healing ♥️
I wish more people talked about miscarriages, and most importantly what comes after! I had two chemical pregnancies prior to this pregnancy, was ELATED when I received a positive heartbeat at 8 weeks, and then earlier this month at my 3-month scan, 4.5 weeks later after my first scan, was told that they could not find a fetal heartbeat, and my baby never made it past 9 weeks from the size. A missed miscarriage. Devastated was an understatement.
The next day, after 24 hours of a lot of tears, I was given the same three options of natural, medical management, and D&C. D&C didn’t make sense for the size, they advised, and the day after my scan my body (ironically) started the natural process. Guess it just needed my mind to know what happened first, who knows.
My OB advised to wait and see how the natural process would go, but gave the prescription from Misoprostol to have just in case. Two weeks later, the natural process still going on, and at a check up with my OB she said if I was still experiencing clotting in a few days, that I could take the Miso and it should “finish things off”. Such a crappy thing to think of, and such a hard decision to make emotionally.
Earlier this week, at the 3rd week of miscarrying, I reached the point that I realized my emotional healing was being delayed by the physical, and opted to take the Misoprostol one night with dinner, approx. 8:30pm. My OB advised to have someone with me, the pharmacist said I would experience some cramping, no one told me exactly what I was in for.
From 10pm to midnight I tossed and turned with intense lower back pain, in and out of sleep. At midnight I was up for an hour in intense pain, bleeding, and other fun stomach issues. After some doses of ibuprofens and a heating pad, I was able to fall back asleep around 1am, only to be woken up at 4:30am in the worst pain of my life. And cue the next 6 hours of 3-minute apart contractions. Experience some cramping? As if! Why did no one tell me it flat out induces labour, and you will experience sudden onset contractions? I guess I also should have done some more research, but I truly wish that the doctor and pharmacist were more forthcoming on what to expect, and to be prepared with proper pain management options.
Was the worst pain I have ever experienced in my life, pretty sure it set me back emotionally, and to boot, still bleeding. I can agree that I would advise anyone in the same situation as me about my experience with Misoprostol, and would likely never opt for it again should I have to make that decision.
Thank you for sharing your story, Kaycie, and I’m so sorry for what you’re experiencing. This is such a brutal and unfair process. I hope you’ll never be faced with this choice again, and I’m so sorry you weren’t better informed. So often, our doctors downplay it, perhaps because they deal with it so often and either haven’t experienced it, or their experience has been dulled by many years? We need to find a way to do much better with patient advocacy and education, for sure. You deserve better. Big, big hugs.