Imagine you’re early in pregnancy, and you feel a twinge of pain on one side of your stomach. What’s your immediate reaction? Very likely, it’s to Google “ectopic pregnancy stories” because we’ve all heard horror stories about ectopic pregnancy.
Knowing that an ectopic pregnancy can mean life or death for the mother, it’s something a lot of us worry about with every early pregnancy pain.
Beth’s ectopic pregnancy story shows that signs of ectopic pregnancy may not always seem obvious.
For many women like Beth, these stories tell of trauma, lost fallopian tubes, and life-saving endeavors.

This site contains affiliate links, meaning that we earn a small commission for purchases made through our site. We only recommend products we personally use, love, or have thoroughly vetted.
What is An Ectopic Pregnancy?
And why the fear around them?
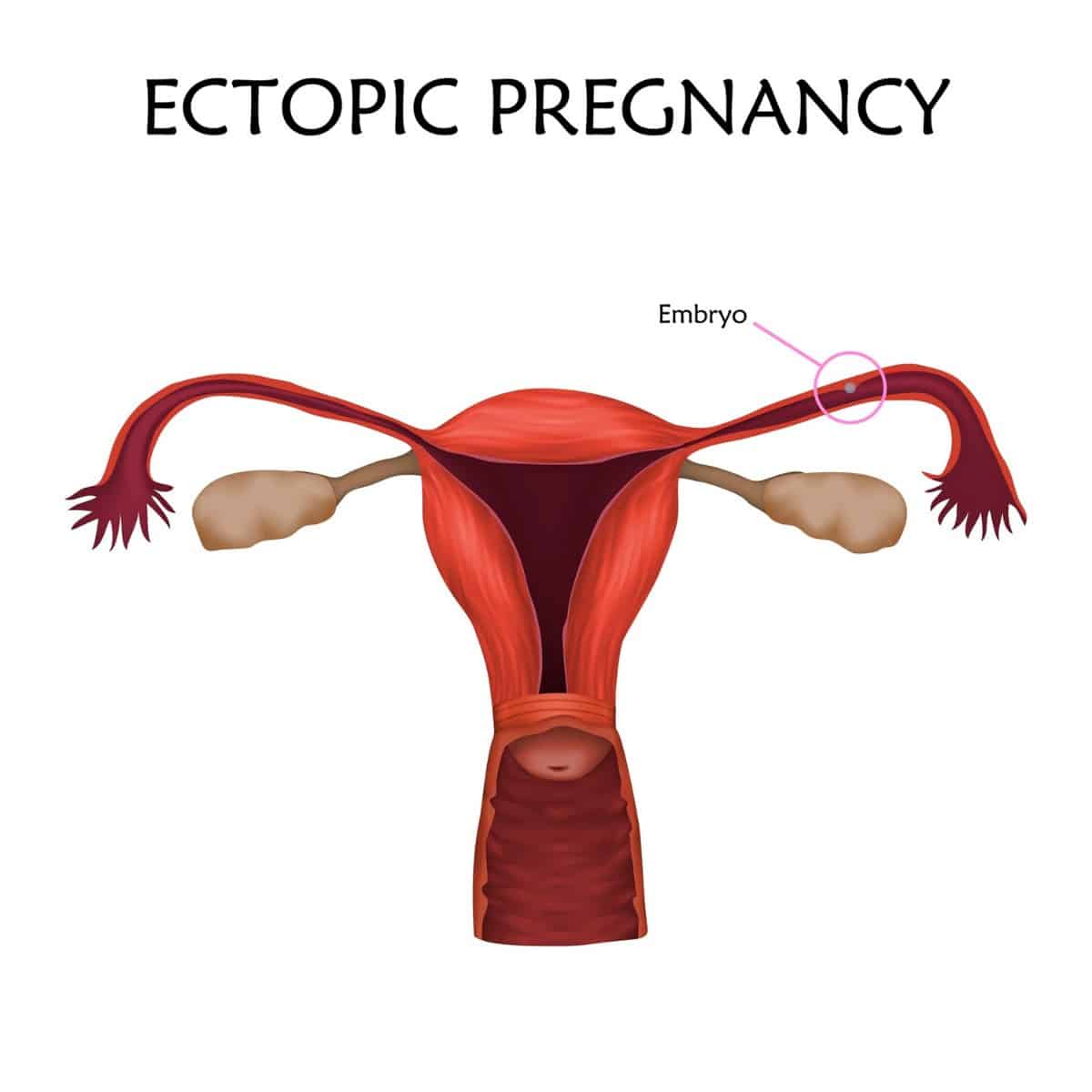
An ectopic pregnancy occurs when a pregnancy never makes it to the uterus. Most often, it implants in one of the fallopian tubes (and is thus commonly referred to as a tubal pregnancy.)
Ectopic pregnancies only occur in about 2% (1 in 50) of pregnancies.
Can A Baby Survive During an Ectopic Pregnancy?
An ectopic pregnancy is never viable.
Once diagnosed, ending the nonviable pregnancy is necessary for the mother’s safety.
Early ectopic pregnancies are often treated with an injection of methotrexate. Women who are further along often require surgery.
Why Is Ectopic Pregnancy Dangerous?
As an embryo grows inside the fallopian tube, it can rupture the tube, causing intense pain and trauma, in addition to a life-threatening condition called sepsis.
OBGYN’s suggest you are much more likely to save your fallopian tube and avoid surgery if you catch an ectopic pregnancy early, which requires knowing the signs of ectopic pregnancy.
What is the First Sign of an Ectopic Pregnancy?
If you experience any of these signs, taken from The American Pregnancy Association, contact your doctor or go to the emergency room immediately:
- Sharp or stabbing pain (may come and go and vary in intensity)
- Pain may occur in the pelvis, abdomen, or even in the shoulder and neck
- Heavier or lighter vaginal bleeding than your normal period
- Gastrointestinal symptoms
- Weakness, dizziness, or fainting
- Low levels of HCG
- Low levels of progesterone
Low levels of HCG and progesterone can only be detected via blood test, so if you have a history of ectopic pregnancy, make sure your OB GYN is monitoring your levels.
Note: an ectopic pregnancy can still present normal signs of pregnancy, such as nausea, breast tenderness, and morning sickness.
Beth’s Ectopic Pregnancy Story: Not the Normal Early Symptoms
Ectopic pregnancy symptoms don’t always manifest in “typical” ways.
I woke up one morning in February happily 8 weeks pregnant. By that evening, everything had changed.
I was in the hospital recovering from emergency surgery. My husband and I had lost our baby. We had sung to that baby every night. We had already started trying to figure out a name.
She or he probably never had a heartbeat. I had an ectopic pregnancy that was now over.
The thing is, I didn’t really have any super concerning symptoms that are usually associated with ectopic pregnancy, such as sharp, stabbing pain in my abdomen. There was no weakness. No fainting.
My ectopic pregnancy story didn’t follow the signs.
Many Early Ectopic Pregnancy Symptoms Mimic Normal Pregnancy Signs
I bled once at around five weeks pregnant and rushed to the ER in a state of panic.
But my HCG (pregnancy hormone) numbers had tripled in three days.
Although I was too early for an ultrasound, my OB reassured me that bleeding can be normal and that all signs pointed to me having a perfectly healthy pregnancy.
A few weeks later, I spotted brown, and my OB again said not to worry. I felt twinges of pain on my side, but was told this is normal as your uterus stretches during pregnancy.
(Editorial note: This is true. Although round ligament pain isn’t said to start until the second trimester, many women report experiencing the same pulling sensation during the earliest weeks of pregnancy.)
The only thing that worried me was that I wasn’t having a lot of typical pregnancy symptoms like nausea, but my OB kept telling me that’s normal for some women. (Again, this is true.)
Then on one awful, painful Saturday, I started bleeding bright red, enough for a pad, in the middle of the morning.
I still didn’t think the pregnancy could be ectopic. I just assumed I was beginning a miscarriage but hoping and praying I was wrong.
A Heartbreaking Trip to the Hospital Saved My Life
The on-call OB from my doctor’s office was SO unhelpful.
He made it perfectly clear that my worst nightmare was simply an interruption to his weekend. (I reported this doctor to my actual OB, who is awesome, at my follow-up a few weeks later).
I began cramping badly. By early afternoon, the cramps were bad enough that I couldn’t concentrate on anything else. I still wasn’t willing to take anything stronger than Tylenol, just in case.
This is when my symptoms became more typical for ectopic pregnancy.
The pain started gravitating to one side and got stronger and stronger as the day dragged on.
I didn’t know for sure, as this was my first pregnancy, but it was what I imagined labor contractions to feel like. But contractions come in waves. This pain was constant.
I couldn’t sit still. I couldn’t sit up straight. Nothing helped.
(Editorial note: Miscarriage, especially after 8-10 weeks, can cause contractions. Much like giving birth, those contractions usually come and go. If your pain is constant, like Beth’s, go to the ER immediately! Learn more about what to expect when miscarrying.)
We finally went to the ER around 6pm. We were only in the waiting room long enough for a nurse to get my symptoms and put a bracelet on my wrist.
An ultrasound confirmed an ectopic pregnancy. My baby, who I had worked so hard to keep safe, never had a chance to survive.
Ectopic Pregnancy Treatment
At first, my doctor gave me the choice between a shot of methotrexate (which dissolves the pregnancy back into the body) or surgery. I had no idea which one was “better.”
Either way, I was losing the most important thing I had at the time: the child my husband and I had dreamed of.
After an hour of deliberating, our doctor decided the amount of pain I was in meant I was probably too late for the methotrexate shot.
To be safe, I needed surgery to make sure my fallopian tube didn’t burst.
My team of doctors ended up removing my right fallopian tube along with my baby, and I was told it was very close to bursting by the time they went in.
My husband just kept saying he was just so glad I was okay after such an intensely close call.
I stayed in the hospital until about noon the next day, until I was able to keep food down and walk around a little.
Then, I was sent on my way with three incisions on my stomach (one larger, one through my belly button, and two smaller ones on either side of my abdomen).

No One Told Me What To Expect with Ectopic Pregnancy
I really had no idea what to expect after my surgery. This is part of the reason we need to talk more about it. Sharing your story can help inform others!
Women going through this heartbreak deserve to know what to expect.
Also, reading others’ stories can be great for mental health when recovering from this physical and emotional blow.
I wasn’t told when I could go back to work or who to call in case of a problem.
No one explained when to remove the big bandage on my belly button, or what to expect when I did.
Nobody mentioned whether the surgical glue would dissolve, or if I needed to do something with it.
I got all of that information from Google, and it took serious digging to figure it out.
If this article can be a resource for even one person who is going through the hell that I went through, then I’ll be happy.
Post-Operative Recovery
For the day or two after surgery, I couldn’t get up on my own.
To get out of a chair or my bed, my husband had to grab my arms and pull my body weight up. I got up only to use the bathroom for the first day or so, and then I was encouraged to start walking again.
I’m extremely lucky my mom is retired and was able to drive four hours to my house (with almost no notice) to stay a full week with us.
My husband was able to go back to work, and I had someone to help me around the house. Plus, it was nice to get to spend some time with my mom after such a harrowing experience.
I took the bandage off of my belly button after a few days, mostly because I was curious what my scar underneath looked like. That scar was still covered in surgical glue, so it was still protected.
The glue took weeks to fall off.
I still had the glue on the big scar when I went back to work 2.5 weeks after my ectopic pregnancy surgery.
If you’re currently recovering from ectopic pregnancy surgery, know that the scar is NOT as big and scary as the glue makes it look.
Do You Bleed After Ectopic Pregnancy Surgery?
I bled for probably the length of a normal period after my surgery. So, a little less than a week.
I bled as my uterus emptied everything it attempted to build for the baby that wasn’t there. Kudos for trying, uterus.
I passed clots, presumably uterine lining my body had been trying to build up to protect the pregnancy. I’ll repeat, though, that my doctors told me nothing. I’m leaning on my own research to make educated guesses here.
I was prescribed Percocet and high-strength Ibuprofen after my surgery, and I finally understand why opioids are so addicting.
Those pills don’t just take away your physical pain; they take away your emotional pain.
People commented that I was very chill in those first few days. I didn’t understand why I wasn’t more upset, given the gravity of what I’d lost.
And then my prescription ran out.
That’s when I finally understood Cristina Yang in Grey’s Anatomy screaming for somebody to sedate her after her own ectopic pregnancy. The physical and emotional pain were strong.
I watched a lot of Netflix, reread the Harry Potter series, hung out with my dog, and just tried to keep myself occupied until I went back to work about two-and-a-half weeks later.
I distracted myself from my miscarriage grief.
Post-Pregnancy Grief
My grieving process was similar to others coping with miscarriage.
I had a meltdown where I threw my positive pregnancy tests around my bedroom and collapsed to the floor.
My husband went home during my surgery to hide the announcement onesie I’d bought on Amazon. He didn’t pull it out until I asked him to months later.
I STILL have no idea where his hiding place is, but I’m determined to find it.
I listened to “Small Bump” by Ed Sheeran probably more times than was healthy. But hey, we do what we gotta do, right?
I’ve noticed how often television uses pregnancy loss as a plot device. Luckily, this doesn’t affect me as much as I expected, but I feel so much for the women it triggers. These scenes are so prevalent, and it sucks.
Telling Friends and Family
We had already told the friends we see regularly that we were pregnant. We were both so excited; we couldn’t keep that to ourselves!
People often ask, “Why is 12 weeks safe to announce a pregnancy?” It’s because miscarriage risk decreases, but for many people, having friends and family know about a pregnancy also helps if a loss occurs.
We were glad our friends and family knew what had happened to us. We had a large support system, and the outpouring of love we received was truly touching. It’s a gift to have friends who know how to support someone after miscarriage.
My husband and I were, and are, so grateful to have had those people in one of the worst times of our lives. Seriously, we have the best friends.
I will never regret telling them about both of our pregnancies because dealing with all of that on our own would’ve been so much harder for us.

Pregnancy After Miscarriage
After one ectopic pregnancy, you’re at increased risk for another. When I became pregnant again in May, my doctor immediately tested my HCG to check on things.
Unfortunately, I miscarried at only five weeks. I have a theory that my body was still trying to heal; it couldn’t heal me and support someone else at the same time.
This explanation helps me better understand two losses in a row, so it’s the narrative I cling to.
Long story short, we’ve had a rough year: two lost babies, one surgical recovery, and a lifetime’s worth of tears and what-ifs. We’ve decided to hold off a little bit before trying again.
When we do get pregnant again, I’m assuming my doctor will have me come in for testing immediately. I’ll advocate for an early placement ultrasound even if the HCG tests are normal.
Because once you lose a pregnancy, you’re absolutely terrified the next time. Pregnancy anxiety after miscarriage is no joke! Every twinge and symptom has you running to Google or a pregnancy blog to make sure it’s normal.
If you’ve had an ectopic pregnancy, know you’re not alone.
Lean on your friends, and family.
Better equip yourself to know the signs, symptoms, and risk factors.
Knowledge can help you through this terrifying experience. You can know your options and advocate for yourself in the ER.
I hope my ectopic pregnancy story can help.
You are not alone.

Risk Factors of an Ectopic Pregnancy
Because risk factors exist before the actual ectopic pregnancy, knowing them can allow you to be extra vigilant.
According to the American Pregnancy Association, risk factors include:
- Maternal age of 35-44 years
- Previous ectopic pregnancy
- Previous pelvic or abdominal surgery
- Pelvic Inflammatory Disease, which is caused by sexually transmitted infection
- Several induced abortions
- Conceiving after having your tubes tied or while an IUD is in place
- Smoking
- Endometriosis
- Undergoing fertility treatments or using fertility medications
If you know that you have any of these risk factors, talk to your doctors before trying to conceive.
That way, you can begin to build a plan of action if you do experience an ectopic pregnancy. Being informed and aware of the risk is the only way to go.
How Long Can You Go With An Ectopic Pregnancy?
Catching an ectopic pregnancy early is key!
If you have an ectopic pregnancy, your fallopian tube is at risk of rupture anytime between 6-16 weeks.
If you believe you’re experiencing an ectopic pregnancy, head to the emergency room immediately for a blood draw and placement scan.
If your doctor cannot tell the location of your pregnancy during a placement scan, advocate for yourself. Ask if a specialist would be able to!
Sometimes, it’s just too early. But specialists often have higher-tech equipment, so they may be able to place your pregnancy when a regular OB and ER cannot.
If you’ve experienced an ectopic pregnancy, tell us your story or symptoms in the comments.
General FAQ About Ectopic Pregnancy
What is an ectopic pregnancy
An ectopic pregnancy occurs when a fertilized egg attaches to the fallopian tube, and for this reason, it is commonly referred to as a tubal pregnancy.
What is the first sign of an ectopic pregnancy?
The first sign is different for everyone, but the most common is sharp abdominal pain or cramps on one side only. If you’re monitoring HCG levels, low or plateaued HCG levels are a common indicator of ectopic pregnancy.
How common is ectopic pregnancy?
Ectopic pregnancies only occur in about 2% (1 in 50) of pregnancies.
Can a baby survive during an ectopic pregnancy?
An ectopic pregnancy is never viable. In other words, it is not possible to have healthy babies from ectopic pregnancies.
How long can you go with an ectopic pregnancy?
It’s best to catch an ectopic pregnancy as early as possible. If you have an ectopic pregnancy, your fallopian tube is at risk of rupture anytime between 6-16 weeks.
How is ectopic pregnancy treated?
Early ectopic pregnancy is usually treated with an injection of methotrexate. Ectopic pregnancies not discovered early often require surgery.
More Miscarriage Stories
Articles about What To Expect When You Miscarry
- Miscarriage memorials
- What to do after miscarriage
- Why you don’t have to attend a baby shower after miscarriage
Other Helpful Miscarriage Articles
- Miscarriage tattoo ideas
- Finding a pregnancy loss support group
- Who is a mother?
- What to say to someone who had a miscarriage
- Pregnancy & Infant Loss Awareness Month
- International Wave of Light
Rainbow Baby Articles
- What is a rainbow baby + what it’s like to have one
- Rainbow baby gifts
Gift Guides
- Choosing the best miscarriage gifts
- The ultimate postpartum care package
- What to put in a new mom care package
- Postpartum + nursing pajamas




I am in the hospital recovering g from my c section scar pregnancy right now. I knew from. My first positive test at 3 weeks 5 days that something was not right. At 4 weeks 6 days I made up symptoms to be seen to rule out ectopic as I was terrified of it. It was too early for ultrasound to show much. Over the next few days my HCG tripled accordingly. My doctor wanted a follow up ultrasound at 6 weeks. To this point,I had no symptoms, other than brown spotting, similar to my three successful pregnancies. On my way to my follow up I had cramps that caused me to pull over and wait for them to pass. I got to the dr and had an Internal scan. I told the ultrasound tech I didn’t want to see anything unless it was a baby with a heartbeat. Eventually she told me to look up,and there was my tiny baby’s heartbeat. As she finished up the scan she said “oh gosh, you are bleeding a lot”. The doctor analyzed the scans and sent us straight to the best hospital around to be treated for CSP. I was given my options and went with the double balloon catheter. I am traumatized and heart broken.
I am so incredibly sorry for your loss, mama. Sending you love!
I am in shock after reading this. So much of this seems to line up with our experience that happened on Oct 11, 2021. We knew nothing! We didn’t even know we were pregnant until I went to the doctor for stomach pain. This extra information that I am reading is incredibly helpful because like Beth, the surgeon, who did not have a practice but is just an on-call for the hospital, was absolutely not helpful at all. Both doctors I saw said I was at 3 weeks, and another at around 5. But with a ruptured tube and apparently a lot of blood in my belly, according to them, I might have beeb later. I will definitely be pushing up my post-op appointment and talking with several doctors about this. I feel like I was just another case late at night and a burden to the doctor.
Thank you for sharing this story. I believe ectopic, from my 2 weeks of research now, gets overlooked and there aren’t many to share out their experiences.
I’m so sorry for your experience! Ectopic pregnancy is so hard and definitely not talked about enough. And unfortunately, in ER scenarios, we often feel like burdens more than people. They’re so busy with trauma, I know, but we’re also experiencing trauma. Sending you love.
I also suffered a miscarriage from an ectopic pregnant at 6 weeks. I had no idea I was pregnant. My last normal cycle had just went away . Started spotting back 3 days later so I went to the ultrasound only to find out i was pregnant in my tube. I was immediately admitted and had surgery
I’m recovering right now from a ruptured ectopic pregnancy. I started spotting on Oct 31st and had 3 positive pregnancy tests. I wasn’t alarmed as I had spotted with my now 7 year old son.
The bleeding became heavier and I thought I had a complete miscarriage on November 12th. The amount of heavy bleeding and clots and loss of symptoms had me believing I had just suffered my 2nd miscarriage in a row. One in 2017 and then now. Because I’m 40, I just assumed it was what it was.
Then during the week of Thanksgiving, I started bleeding heavily again and felt the symptoms of pregnancy so I took another test and it was positive. I was stunned. I was also beginning to have a lot of lower pelvic pressure and eventually pain that was so bad I couldn’t stand up straight. I took Motrin and because it was a Holiday, my doctor asked if I was running fever which I was not and said I should be fine to wait until my appointment that was scheduled for December 18th.
November 30th, I was working at my home office and fainted. My husband called for an ambulance and I remember not being able to breathe in the ER.
I could barely stay conscious while the ultrasounds were done. I was given no pain medicine the entire time I was waiting for surgery.
The doctor told me the fetus was still living in my tube and it would be removed along with my left ovary. I too, was told that I had a lot of blood in my stomach and they tried to wash it out, but couldn’t get it all out. I had lost almost 2 liters of blood and have to have a transfusion after surgery.
I am on day 4 after my surgery. I’m in pain. I do have some bleeding, similar to a period. My doctor told me if I had waited any longer I would not have survived. She saved my life, but it’s also very clear that ectopic pregnancy can be very sneaky and life threatening.
I haven’t been told when I can return to work. I’ve just decided that I will return Monday, since I do work from home. I hope my experience helps any others that are trying to decide whether to get to the ER or wait. Don’t wait. It’s just not worth it.
On February 7th 2022 I had a ultrasound for a non related matter, to me every thing seemed normal except the nurse was really quiet. A hour and a half goes by and the nurse tells me to wait in the waiting room but had no response when I asked why. A half hour later the same nurse came to me and brought me into the emergency room where I was asked to sign in AGAIN and at this point I was overly angry and confused. After signing in a nurse brought me to a room and told me my baby was in the fallopian tube , that’s when I found out I was pregnant!. After some tests I was told their was not only one but two and I was 6 1/2 weeks along and they had a heart beat. I was told their placement was at the corner of my uterus and at the opening of my left fallopian tube so they had to surgically remove them the whole tube including a part of my uterus , this scared me because not only is this my first pregnancy but my first surgery and with twins !! I was transferred to the nearest major hospital where I spent the next three days trying to wrap my head around everything that was going on but it never felt real. The morning of surgery I had another ultrasound to double check on the situation and I was informed their hears had stopped, I tried convincing my self it was a blessing in disguise because if they had gotten any bigger my life would be more at risk .once I saw two little grains of rice in a big egg it hit me I was almost a mom and I was about to have surgery. I think the worst part was knowing Even if I wanted to continue on with the pregnancy I still had no choice but to end it. A few days later I am still trying to cope with this traumatic situation, but both god and I know I am not ready for kids nevermind twins and I know one day he will give them both back to me at some point in my life.
Thank you so much for posting this. Same story, 12 weeks, ruptured. 5 ‘medical professionals’ told me not ectopic; glad I advocated. Sending positive vibes. Thank you again.
I had the unfortunate luck of having 2 ruptured ectopic pregnancies 15 mos apart. Lost both tubes now. Both babies. Both had no pregnancy symptoms but out of nowhere searing abdominal pain that i couldn’t get comfortable with, cold sweats, and shoulder pain from the blood in my abdomen. The first one i lost 2 L of blood from puking with pain meds, no transfusion, high iron pills, and went back to work at 6 weeks. This one i lost almost a L, no pain meds so no puking, iron pills, and idk when I’ll go back to work yet since my post op is in a week. The grief is pretty hard and explaining it to my almost 12 year old who has been begging for a sibling for her entire life is devastating. Also explaining to your husband that you feel like a broken woman is gut wrenching. My heart goes out to anyone who has been through this but especially in this post Roe v Wade world.