When I lost my first pregnancy, a blighted ovum, I was blindsided by the news. I knew little about pregnancy loss at the time, but my understanding was that losing a pregnancy meant I would experience heavy bleeding and cramping. I never knew that I could feel perfectly normal walking into a doctor’s office, only to find out that, despite no symptoms, I was experiencing a missed miscarriage.
Missed miscarriages are called by various names. It’s possible your doctor will refer to it as a “silent miscarriage,” “missed abortion,” or “silent abortion.” If you hear the latter phrases and they’re hurtful, I hear you, I’ve been you, and I’m here for you. “Abortion” is the medical term for miscarriage, so it’s something you might hear when you’re experiencing the loss of a wanted pregnancy.
Unfortunately, missed miscarriages aren’t something many of us know much about, so I’ll tell you everything you need to know to help you move through the process and make all the hard decisions.
This article will include answers to your major questions about missed miscarriage, including:
- What is a missed miscarriage?
- Are there missed miscarriage symptoms?
- How is a missed miscarriage diagnosed?
- What are my treatment options?
- How do I choose the best missed miscarriage treatment for me?

This site contains affiliate links, meaning that we earn a small commission for purchases made through our site. We only recommend products we personally use, love, or have thoroughly vetted.
What is a missed miscarriage?
A missed miscarriage is the loss of a pregnancy that occurs without the mother knowing about her loss. There are many different types of miscarriage, but this one often surprises women who expect all losses to begin with cramping and bleeding.
According to the American Pregnancy Association, a missed miscarriage occurs when “when embryonic death has occurred but there is not any expulsion of the embryo.”
In other words, the pregnancy stops developing, but the mother does not bleed or cramp, and thus does now know there’s a problem with the pregnancy.
What are the signs of a missed miscarriage?
One of the hardest parts of a missed miscarriage is that there aren’t really typical signs of miscarriage. According to the Miscarriage Association, “There is often no way you could know, except by having an ultrasound scan.”
Of course, this lack of knowledge leaves many of us in terror as we walk into each ultrasound appointment, but the odds are in your favor.
Only 1-5% of pregnancies ends in a missed miscarriage. Of course, if you find yourself on the wrong side of these odds, the word “only” carries no weight.
Many women in the pregnancy loss community worry about miscarriage when their pregnancy symptoms dissipate. While this anxiety is understandable, as decreasing HCG levels (the pregnancy hormone) can cause a loss of symptoms, many people’s pregnancy symptoms decrease around week 12, and it’s not uncommon for symptoms to decrease much earlier.
When I experienced a missed miscarriage, I actually had worse pregnancy symptoms than during my successful pregnancy.
With a missed miscarriage, it’s possible for HCG levels to continue increasing and even for the uterus to continue growing until your body recognizes the loss.
How is a missed miscarriage diagnosed?
Because there are no reliable symptoms, a missed miscarriage is diagnosed by ultrasound. I know this is frustrating, but unfortunately, there’s no other medical way to diagnose a missed miscarriage.
In this next section, I will explain the varying types of missed miscarriage, including blighted ovums and when the embryo stops developing.
Blighted ovum
Early missed miscarriages are often the result of a blighted ovum (also called an “anembryonic pregnancy”).
According to the American Pregnancy Association, a blighted ovum occurs “when a fertilized egg attaches itself to the uterine wall, but the embryo does not develop. Cells develop to form the pregnancy sac, but not the embryo itself.”
When I experienced a blighted ovum, my gestational sac continued to grow and my HCG levels continued to rise. I learned at one ultrasound appointment that there was a chance I was miscarrying (often called a “threatened miscarriage”), and a scan a week later confirmed my loss.
I want to make one point very, very clear. If you’re experiencing this type of pregnancy loss, your emotions are valid. You were pregnant. A problem occurred like in any other miscarriage. And you’re allowed to feel whatever you need to feel.
It’s common after a blighted ovum for people to say hurtful things like, “At least there wasn’t really a baby.” But let me tell you something, mama. A sperm and egg came together and began forming. You saw a positive pregnancy test. You dreamed of a life. Now that life has been stolen from you. It’s okay to grieve.
And if you would consider saying this to someone experiencing this type of loss, please learn what not to say to someone who had a miscarriage.
When the embryo stops developing
Most missed miscarriages that occur before a heartbeat is detected are blighted ovums, although there are certainly instances of losses where the embryo did begin to develop and then stopped developing.
Whether you’re learning of your missed miscarriage before or after you heard a heartbeat, whatever emotions you experience are valid.
But when you’ve heard your baby’s heartbeat and you thought all was well, hearing a quiet ultrasound room can be the most deafening silence you’ve ever imagined.
I’m so sorry; please know we’re here to support you, and you are not alone Read other missed miscarriage stories.
Missed miscarriage treatment options
I have a lot of ambivalence about missed miscarriage treatments, and the fact that you have options if you’re experiencing this type of loss. Part of me found a lot of comfort in the fact that I had choice–at least something in this uncontrollable process was within my control.
Then again, having to make a choice is hard, especially when you’re already grieving and can’t see a clear path forward.
I’ll walk you through your three major treatment options for a missed miscarriage, including the pros and cons of each.
It’s worth nothing that, if you discover your missed miscarriage during very early pregnancy, it’s possible that you have a fourth option to dissolve the pregnancy with an injection of methotrexate.
The only way you’re likely to know early enough, though, is if you’re being monitored by a reproductive specialist who does a placement scan at 5-6 weeks. For the vast majority of women experiencing a missed miscarriage, this is not a viable option.
(1) Medication: Cytotec/Misoprostol
Cytotec is a pill you can take to help induce miscarriage naturally. Also called misoprostol (the generic form), this medication can be taken orally or inserted vaginally, depending on the instructions given by your doctor.
The idea is that misoprostol induces miscarriage, but you still get to go through the process naturally, hopefully without waiting. For many women, this process works well and they report no problems.
For others, though, taking misoprostol can be a very traumatic experience with very intense pain and bleeding. Arden’s misoprostol experience is one such story.
When I had my Dilation and Curettage (D&C), the OR nurse told me that 50% of people who take misoprostol end up requiring a D&C for incomplete miscarriage. Arden’s doctor told her the number is 60%. But we do not have research to support those numbers; we are simply reporting what care providers have told us.
I do personally know many women who have taken Cytotec successfully, and they do not have nearly the hospital bills that women who need a D&C are faced with.
Note: Have someone on hand to monitor your bleeding in case it requires an emergency room visit. Please call your doctor if you’re concerned about the amount of bleeding. Go to the ER if you soak through more than one pad per hour.
(2) Surgery: Dilation & Curettage (D&C)
A D&C is a surgery in which you are fully sedated while your doctor dilates your cervix and removes all of the contents from your uterus.
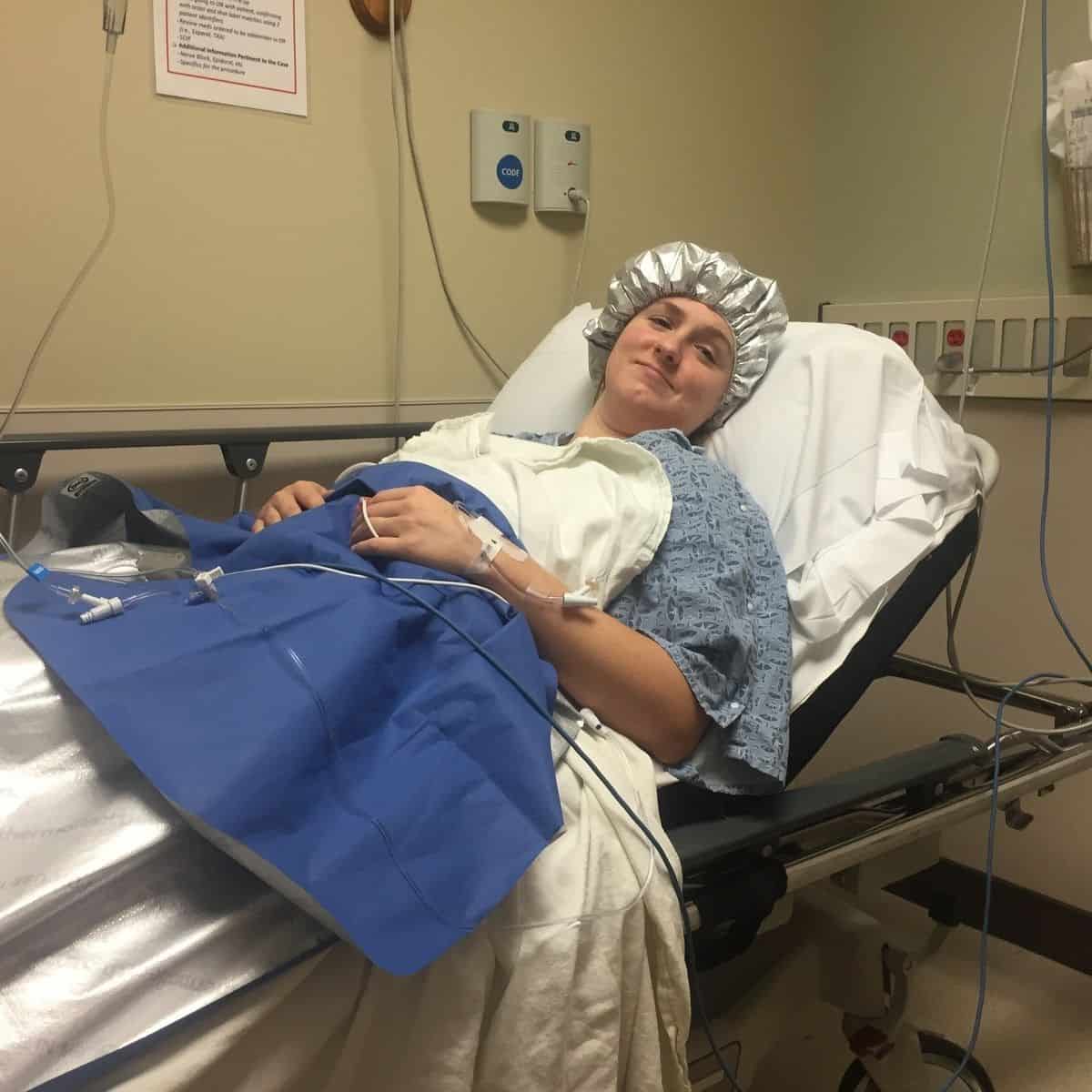
I elected for a D&C after my missed miscarriage because the process felt the most controlled to me. I would go to sleep, wake up, and be able to begin the physical and emotional process of healing. And honestly, it really was that simple.
But a D&C procedure is not without its drawbacks. Depending on your location, it can be quite expensive, which feels like a massive punch in the gut when you’re losing a wanted pregnancy.
Also, there are risks. While most D&Cs cause no complications, it is possible to develop infection or Asherman’s Syndrome, both serious conditions.
Note: After a D&C, you may opt to have the pregnancy tissue tested for genetic abnormalities, which may help you identify how to best manage future pregnancies. This option can be expensive, though, and is not guaranteed to provide answers. Talk to your health care provider to determine the best choice for you.
(3) Wait to miscarry naturally
Although options 1 and 2 are relatively interchangeable in terms of which is “better” because they each fit different situations differently, I put this option last for a few reasons.
If you choose to wait to miscarry naturally and have your doctor’s approval, it could be a really great option for you.
But there are a few reasons I recommend against this approach.
First, there’s a really strong emotional toll of knowing you’re carrying a pregnancy that isn’t progressing. For most women, that’s too much to put themselves through.
Second, there are physical risks that come with waiting to miscarry. Specifically, infection.
One of our community members told me the story of waiting to miscarry naturally after her missed miscarriage. She spent 9 weeks waiting to miscarry, during which time she suffered various signs of infection, including high fever and chills.
Untreated infection can lead to sepsis and cost miscarrying moms their lives, and this community member was lucky to come out of the ordeal physically unscathed, though emotionally very harmed.
I don’t tell this story to scare you. Obviously, 9 weeks is a long time to wait, and the fact that her care provider did not step in is mind-boggling to me.
Rather, I tell you this story to say that, if you and your care provider choose to wait to miscarry naturally, please make that choice with careful and regular monitoring. It might be that your body recognizes the loss soon, but it also might not.
Being supervised by a medical professional is CRUCIAL if you decide to miscarry naturally.
How to choose the best treatment option for you
The best treatment option for you depends very much on your location, circumstances, and care provider.
In the US, if you don’t have health insurance, a D&C will likely be a great expense. Even with health insurance, it can end up costing thousands of dollars out of pocket, which is far more than most of us are prepared to spend to lose a wanted pregnancy.
Read more about the financial and emotional cost of miscarriage.
The cost will vary at different hospitals and with different insurance providers, so talk to your doctor about whether surgery is a reasonable option for you.
Another question to ask yourself is whether you want the closure of a physical miscarriage.
I elected for a D&C because it felt the most controlled, and I wanted to feel in control of something. Taking misoprostol would have sent me into a whole new world of unknowns.
That said, many miscarrying moms report a preference for misoprostol because they need the closure that comes from physically expelling a pregnancy.
Discuss your finances and what you think will be best for you emotionally with your care provider. If you’re clear on the choice you want to make, advocate for your care provider to honor that choice.
What missed miscarriage treatment option did you choose? Tell us about your experience in the comments.
Common questions about missed miscarriage
If you elect to have a D&C, the miscarriage will be over after surgery. If you elect to take misoprostol, or miscarry naturally, the amount of time that it takes your body to miscarry will vary from person to person.
It is incredibly important that your care provider monitor you during a miscarriage. If a miscarriage is not removed, or is “incomplete,” you may incur serious infection, which could lead to sepsis.
Research suggests that 1-5% of pregnancies result in a missed miscarriage.
Because the body does not recognize the loss of a pregnancy during a missed miscarriage, it is often difficult to tell when one has occurred as signs or symptoms don’t really exist for most women. An ultrasound scan is the only way to confirm a missed miscarriage.
More Miscarriage Articles
- What to expect when miscarrying
- How to deal with miscarriage
- Coping with miscarriage grief
- Miscarriage support groups
- Books about miscarriage
- Creating healing miscarriage memorials
- How to get out of a baby shower after miscarriage
- Miscarriage ornaments
Miscarriage Stories
- Beth’s ectopic pregnancy story
- What it’s like miscarrying twins
- Miscarriage after an unplanned pregnancy
- Whitney’s story of back-to-back miscarriages





