I was 36 1/2 weeks pregnant when I found out I’d have an induced labor at 37 weeks. It was a Wednesday, and my high risk specialist confirmed a preeclampsia diagnosis that we’d expected for weeks.
But I was completely unprepared–scratch that, absolutely terrified–when she said I had 4 days to get everything in order (while on modified bed rest) before checking into the hospital for induction.
Have you just found out you’re having labor induction at 37 weeks of pregnancy? If so, I’m here to share my story and calm your nerves. I did lots of research, as I do, and no worries, mama–all went very well.
I’m a control freak, and after surviving recurrent miscarriage, I could not handle knowing that I’d lost control of my body and birth experience.
Yet I realized I HAD to accept the reality an early induction–I knew enough about Downtown Abbey to know what preeclampsia could do if not carefully monitored (which, of course, mine was).
And so I found something I could control.
I couldn’t control preeclampsia. Or the fact that I was having an induced labor at 37 weeks. Or the fact that my house was still under construction when I got this news. Nope. All out of my control.
What I could control, at least to an extent, was how the induction went.
I knew far too many people whose induced first labors had stalled and lasted days.
I decided to research and do everything I could to make it go smoothly and quickly. Induced labor can be a scary thing, but it doesn’t always have to be.

This site contains affiliate links, meaning that we earn a small commission for purchases made through our site. We only recommend products we personally use, love, or have thoroughly vetted.
- Watch My 37 Week Induced Labor Story
- Why have a labor induction at 37 weeks?
- What to expect from an induced labor at 37 weeks
- What to Expect at the Hospital: My Story
- Inducing labor with pitocin
- More Pregnancy Articles
- More Childbirth Articles
- Articles for New Parents
- Other Favorites from Undefining Motherhood
Watch My 37 Week Induced Labor Story
Want to hear all about my experience? I share it all in this video.
Why have a labor induction at 37 weeks?
Inducing this early is not the norm, and it is not recommended by the American College of Obstetricians and Gynecologists (ACOG) unless continuing to carry the pregnancy could post a risk to the mother or baby.
According to the Mayo Clinic, these reasons could include:
- Gestational hypertension (high blood pressure caused by pregnancy)
- Preeclampsia (the reason I was induced early)
- Your water has broken but you haven’t begun actively laboring, thus you’re losing fluid from your amniotic sac
- Uterine infection
- Fetal growth restriction
- Oligohydraminos (not enough amniotic fluid)
- Gestational diabetes
- Placental abruption
There can be other medical causes, but these are the most common. It’s not recommended to induce labor at 37 weeks without a medical cause.
What to expect from an induced labor at 37 weeks
If you’re being induced this early, your doctor will likely do what they can to prepare your baby for induction.
While your baby is technically considered full-term at this point, there are still things that are developing in its little body. Particularly, the lungs, brain, jaw, and feeding reflexes.
Many doctors will give you two steroid injections prior to labor, with each injection being 24 hours apart. These injections help baby’s lungs develop, and while they are often lifesaving for babies born preterm, they can still make a big difference in your baby at 37 weeks.
Then you’ll likely be left to rest and prepare for induction day. Your OB or high risk specialist may also monitor you using non-stress tests, or other procedures depending on the medical reason for your induction.
At this point, you’ll want to have your hospital bag essentials packed and ready to go. Take them with you to all doctor’s appointments, because it’s possible you could be induced even earlier if anything at the appointment appears abnormal.
(Not sure what to pack? Download our printable hospital bag packing list!)
What to Expect at the Hospital: My Story
My hospital had me come in the night before my induction, so I technically went to the hospital at 36 weeks, 6 days. They told me I would go in that day, but that they’d call me sometime during the day with a check-in time, determined by the availability of beds.
Husband and I grabbed my favorite dinner with the best queso in Atlanta, and I couldn’t eat a bite because I was so nervous. Then, we checked into the hospital.
That night was quiet. They gave me a cervical ripening agent (inserted directly into the vagina) before I went to bed in hopes that it would induce labor on its own, but warned me that Pitocin would likely be necessary the next morning.
They were right.
*Note: The most commonly used cervical ripening agent is cytotec, which is also commonly used to induce miscarriage. I had too much trauma about the idea of using this drug based on my history with recurrent miscarriage. If this will potentially upset you, ask your doctor to use a different option. There are different options!
Then we went to sleep and woke up at 6am to eat breakfast before they started my Pitocin drip at 7am.
Other interventions that are possible
In addition to the use of a cervical ripening agent and a Pitocin drip to cause labor to start, it’s possible that you’ll need help with your water breaking or with actual delivery.
Talk to your doctor (and your support person) ahead of time about your feelings about things like:
- Scraping the membranes to help speed induction
- Breaking your water manually
- Pain management options that aren’t as strong as an epidural
- Use of episiotomy or foreceps during delivery
- C-section
Inducing labor with pitocin
There are always risks with any medication, but on the whole, the major difference between a labor your body induces naturally and one induced with Pitocin is the strength of the contractions.
Women who labor with Pitocin-induced contractions report stronger, more painful contractions and are more likely to get an epidural.
This was my story, although I had always planned to birth with an epidural.
Because I was being induced at 37 weeks, I actually chose to hold off on the epidural for longer because I feared my labor would stall.
Knowing that induced labor tends to last longer than natural labor, and that induced first births tend to last much longer, I determined that I would do everything I could to push through my birth. Pun not intended.
Keep it moving with wireless monitors
My research taught me that moving around throughout labor, especially early labor, could help prevent it from stalling. In fact, specific movements can even start a stalled labor back up.
I strongly encourage this approach to anyone who’s anxious about an induced early labor.
As I learned, and my medical team confirmed, freedom of movement in labor is a great way to take control of your pain and “use gravity to help your baby come down and increase the size and shape of your pelvis.”
Before the nurse starts your pitocin drip, ask for wireless monitors. Insist upon wireless monitors.
Hospitals keep fetal monitors strapped to you during labor to ensure neither mom nor baby experiences fetal distress.
But traditional monitors will keep you hooked to a machine and, thus, stuck in bed. Laboring while still through Pitocin-induced contractions is no joke!
You’ll want to be able to move, and wireless monitors will give you that freedom.
Bring comforting labor tools
We learned in our birthing class that having your partner or support person rub your low back with a massager can help mama manage contractions.
So of course I ordered every massager Amazon had to offer. I was determined to stand and walk through early labor to ensure it didn’t stall.
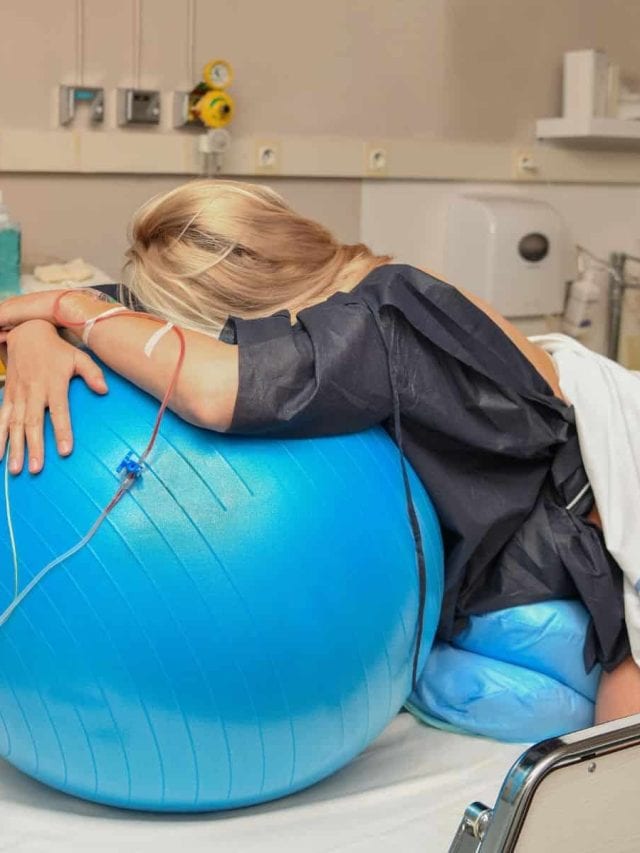
I also took a birthing ball, and I signed the waiver to be allowed to sit on it, although I never did. Instead, I put it on a countertop and leaned into it, dancing with it through the pitocin-induced contractions.
While I danced, Husband tested out each massager on my low back. (Naturally, I hated all the fancy ones and would only let him near me with the most basic, plastic one I could find).
By God, if I had to have my baby by induced labor 3 weeks early, I was going to move!
Advocate for Yourself
Going into your induced labor knowing what to expect and what you want is critical. But also, make sure your support person knows what you want so you can both advocate for your needs.
As soon as I checked into the hospital, I said to the nurse, “I need wireless monitors. I want to walk.”
“That won’t happen until morning,” she assured me, but I insisted. I needed them in my room. I had to know they were there.
We fought over it, but she ultimately refused (and logically so, given that there were likely women in active labor that night who needed those monitors).
First thing in the morning, when I knew my labor was about to be induced, I immediately rang the nurse’s button. “I need my wireless monitors now.”
There was a shift change happening, and the new nurse would come in to start my pitocin drip. She would handle it, I was told.
Induced Labor Control Freak Monster
But the new nurse didn’t immediately agree to bring me the monitors either.
“We need to keep you on traditional monitors for now,” she responded to my demand. “But when your labor progresses to a point that you need to get up, I promise I’ll get them for you.”
The new nurse would become one of the people I’m most thankful for, but in this moment, I breathed fire at her.
Nope. Not this time, lady.
I was freaking resolute. There was about to be something the size of a watermelon canon-balling out of something the size of a lemon. SHE WOULD BRING ME THE DAMN WIRELESS MONITORS.
“Are there any available right now?” I asked.
There were.
“Then bring them in here. I have to have them. I have to know I have them.”
She recognized the animal ferocity in my eyes and placed two on the table right beside me. Within 2 hours, I was hooked up to wireless monitors and walking around, Pitocin drip in tow.
Had I needed to remain in bed connected to traditional monitors, I’d have had an epidural much sooner. The movement so tremendously helped the pain, and I’m confident it hastened my labor process.
After the epidural
I finally got an epidural at 6cm. I took a nap, watched some TV, talked to Husband, and then learned how it felt to think your pelvic bone might shatter.
Jack’s head was pushing down. My induced labor had not stalled.
*Note: What I wish someone had told me about an epidural. You may not feel pain, but you can still feel pressure. And eventually, pressure can be worse than pain.
I asked the nurse about the pressure. She said that, when it stopped being intermittent, that’s when I was ready to push.
I took this advice entirely too seriously and turned into my stubborn self, constantly refusing to push the call button despite imagining how many bone fragments would be floating around if my pelvic bone burst like glass.
I swear I could’ve had Jack 2 hours earlier if I’d known to ask the nurse to check my cervix.
Finally, Husband pushed the call button for me. Thank God for Husband. I reiterate: your support person should be willing and able to advocate for you.
The nurse checked my cervix. When I heard her say, “Whoa,” I excitedly asked, “Am I at 10 centimeters yet?”
“You’re way past measuring your cervix, sweetie,” she told me. “It’s long been pushed up behind his head. I see nothing but a lot of head.”
WHAT?
“DON’T PUSH!” she said to me. “The doctor has to be here to catch the baby. I’m not allowed to. I’m calling her right now.”
Can You Say “Oops?”
30 miserable minutes later, my doctor finally arrived, and within minutes, so did my beautiful baby, Jack.
(I mean, he was sort of beautiful. He also sort of looked like an alien. Let’s be honest with each other about how not pristine vaginally birthed babies are.)

He was healthy, happy, breathing (something I had never been certain could actually happen to a baby of mine.)
There he was, all alien-like, proving all my negative experiences and worst fears wrong.
The nurse who began my pitocin at the beginning of her shift helped me push Jack into this world at the very end of it. I wish I remembered her name. I can see her face. She was a Godsend.
She never believed I’d have a first labor–an induced labor at 37 weeks at that–in just 12 hours. When it happened, she leaned in to me and whispered in my ear.
“I hope you know that you made this happen. You did your research, you trusted your body, you advocated for yourself. You should be really, really proud.”
I will forever love that nameless woman whose face I will never forget. But even if she hadn’t been willing to bring me the wireless monitors, I would have found someone who would.
Interested in other labor stories?
Read this first baby labor story, or check out Chase’s labor story AND learn the benefits of patient empowerment!
More Pregnancy Articles
- Pregnancy planner
- Pregnancy pillows
- Cute maternity clothes
- Pregnancy essentials
- Baby registry must haves
- Best labor and delivery gowns
- When to go to the hospital for labor
- Push present ideas
More Childbirth Articles
Articles for New Parents
- Men’s diaper bags
- Best diaper bag backpack
- Best baby pajamas
- Postpartum must haves
- Baby’s first Christmas ornament










Thanks for sharing your story and your tips! I’m having an induction with my second at 39 weeks (if she doesn’t come sooner) so I’m hoping to use some of these ideas. However, I wanted to let you know I just recently learned that wireless monitors are not always an option. I asked my OB about them and she said that, as far as she knows, they don’t have those AT ALL anywhere in the area where we live (which is fairly rural, but not THAT rural)! I was shocked! I am hoping to still be able to sit/stand/ move a little, but obviously it will be very limited with consistent wired monitoring. Thanks again, Katy!
Thank you for letting me know this! I’ve talked to many OBGYNs who have emphasized how helpful wireless monitoring can be, but no one has ever suggested they aren’t available in most hospitals.
Currently lying in a hospital bed not sleeping at 5 am as I am being monitored for high blood pressure and going to be induced in a couple days…… trying to wrap my head around everything…. Taking SO MUCH ENCOURAGEMENT from this post. What a blessing. Thank you for sharing.
I’m so grateful my story is supporting you! You’ve got this, mama!